Slides and Transcript
Slide 1 of 23
In this section, we’ll be talking about antidepressant-induced sexual dysfunction, the mechanisms and prevalence.
Slide 2 of 23
People have tried to look at where in the brain these problems may occur especially associated with medications. So in a study looking at imaging and antidepressant-associated sexual dysfunction, 18 non-depressed heterosexual men received 20 mg of paroxetine, 150 mg of bupropion or placebo for seven days each in a randomized crossover design. There was a week in between all doses in which these men did not receive any medications. They viewed erotic and non-erotic stimuli in a randomized double-blind within-subject design with serial fMRIs.
References:
- Abler, B., Seeringer, A., Hartmann, A., Grön, G., Metzger, C., Walter, M., & Stingl, J. (2011). Neural correlates of antidepressant-related sexual dysfunction: A placebo-controlled fMRI study on healthy males under subchronic paroxetine and bupropion. Neuropsychopharmacology, 36(9), 1837-1847. https://doi.org/10.1038/npp.2011.66
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 3 of 23
When men viewed the erotic video on placebo, the activated anterior cingulate cortex, the amygdala and the hypothalamus showed up versus the activity seen on the non-erotic stimulus. Paroxetine decreased brain activation in multiple areas of the ACC, the mid-cingulate and midbrain structures such as the nucleus accumbens and ventral striatum versus placebo.
References:
- Abler, B., Seeringer, A., Hartmann, A., Grön, G., Metzger, C., Walter, M., & Stingl, J. (2011). Neural correlates of antidepressant-related sexual dysfunction: A placebo-controlled fMRI study on healthy males under subchronic paroxetine and bupropion. Neuropsychopharmacology, 36(9), 1837-1847. https://doi.org/10.1038/npp.2011.66
Slide 4 of 23
While when they received bupropion, increased activity in these areas was seen plus increased activity in the amygdala and thalamus greater than either placebo or much greater than paroxetine.
References:
- Abler, B., Seeringer, A., Hartmann, A., Grön, G., Metzger, C., Walter, M., & Stingl, J. (2011). Neural correlates of antidepressant-related sexual dysfunction: A placebo-controlled fMRI study on healthy males under subchronic paroxetine and bupropion. Neuropsychopharmacology, 36(9), 1837-1847. https://doi.org/10.1038/npp.2011.66
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 5 of 23
So it appears that paroxetine has negative effects on various brain areas related to viewing an erotic stimulus. Whereas, bupropion shows increases in activity in those areas thereby potentially enhancing sexual function.
References:
- Abler, B., Seeringer, A., Hartmann, A., Grön, G., Metzger, C., Walter, M., & Stingl, J. (2011). Neural correlates of antidepressant-related sexual dysfunction: A placebo-controlled fMRI study on healthy males under subchronic paroxetine and bupropion. Neuropsychopharmacology, 36(9), 1837-1847. https://doi.org/10.1038/npp.2011.66
Slide 6 of 23
Genetics have also been evaluated for looking at an association with sexual dysfunction. In a study involving 81 individuals ages 18 to 40 years who did not have sexual dysfunction at baseline, were assessed for sexual dysfunction with the CSFQ when started on SSRIs for MDD.
References:
- Bishop, J. R., Moline, J., Ellingrod, V. L., Schultz, S. K., & Clayton, A. H. (2006). Serotonin 2A -1438 G/A and G-protein Beta3 subunit C825T polymorphisms in patients with depression and SSRI-associated sexual side-effects. Neuropsychopharmacology, 31, 2281-2288. https://doi.org/10.1038/sj.npp.1301090
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 7 of 23
The serotonin 2A-1438 GG genotype was associated with sexual dysfunction in patients with MDD on an SSRI versus those who had the GA or AA genotype. The GG genotype was a significant predictor of lower arousal scores particularly in women.
References:
- Bishop, J. R., Moline, J., Ellingrod, V. L., Schultz, S. K., & Clayton, A. H. (2006). Serotonin 2A -1438 G/A and G-protein Beta3 subunit C825T polymorphisms in patients with depression and SSRI-associated sexual side-effects. Neuropsychopharmacology, 31, 2281-2288. https://doi.org/10.1038/sj.npp.1301090
Slide 8 of 23
In another study of 115 outpatients also aged 15 to 40 years on SSRIs for MDD assessed for sexual dysfunction with the CSFQ, the SLC6A4 promoter region for the serotonin reuptake location, that insertion-deletion variant was associated with sexual dysfunction and gender differences were found in the study related to oral contraceptive use.
References:
- Bishop, J. R., Ellingrod, V. L., Akroush, M., & Moline, J. (2009). The association of serotonin transporter genotypes and selective serotonin reuptake inhibitor (SSRI)-associated sexual side effects: possible relationship to oral contraceptives. Human Psychopharmacology: Clinical and Experimental, 24(3), 207-215. https://doi.org/10.1002/hup.1006
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 9 of 23
So LL genotype females had an eight-fold greater risk of sexual dysfunction than non-oral contraceptive users. So we should be thinking about women who are on oral contraceptives as that potentially being related to their sexual dysfunction as well as potentially their antidepressant medication.
References:
- Bishop, J. R., Ellingrod, V. L., Akroush, M., & Moline, J. (2009). The association of serotonin transporter genotypes and selective serotonin reuptake inhibitor (SSRI)-associated sexual side effects: possible relationship to oral contraceptives. Human Psychopharmacology: Clinical and Experimental, 24(3), 207-215. https://doi.org/10.1002/hup.1006
Slide 10 of 23
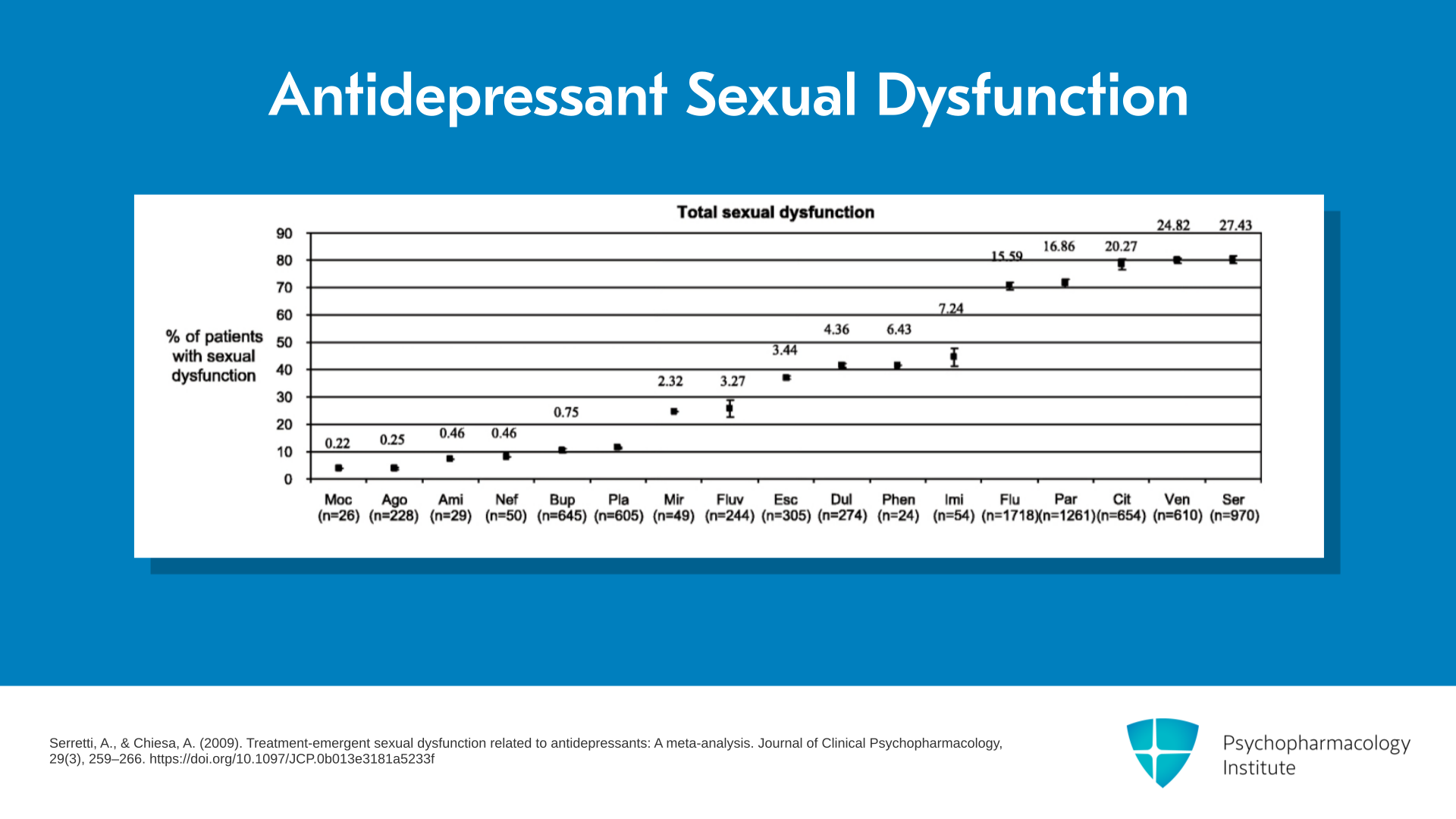
Serretti and Chiesa did a meta-analysis looking at the prevalence of antidepressant-associated sexual dysfunction in the literature. Here, you can see placebo as fourth from the left as the comparator. And three agents showed lower rates than placebo including bupropion, nefazodone and agomelatine. In this middle group, it’s mostly composed of SNRIs and tricyclic antidepressants which have midway effects. About 45% of patients had sexual dysfunction on these medications. And here to the right, you can see a whole group of SSRIs and venlafaxine which is an SRI only up to doses above 150 mg daily. And these rates are about 70% of patients taking an SSRI or venlafaxine having sexual dysfunction. These are shocking numbers and should be addressed.
References:
- Serretti, A., & Chiesa, A. (2009). Treatment-emergent sexual dysfunction related to antidepressants: A meta-analysis. Journal of Clinical Psychopharmacology, 29(3), 259–266. https://doi.org/10.1097/JCP.0b013e3181a5233f
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 11 of 23
One of the ways we can do that is to potentially put patients on from the beginning or change them to antidepressants that are less likely to have sexual dysfunction as an adverse effect. We’ve mentioned already SSRIs, venlafaxine, tricyclic antidepressants and oral MAOIs as causing these kinds of sexual dysfunction.
References:
- Serretti, A., & Chiesa, A. (2009). Treatment-emergent sexual dysfunction related to antidepressants: A meta-analysis. Journal of Clinical Psychopharmacology, 29(3), 259–266. https://doi.org/10.1097/JCP.0b013e3181a5233f
- Higgins, A., Nash, M., & Lynch, A. M. (2010). Antidepressant-associated sexual dysfunction: impact, effects, and treatment. Drug, Healthcare and Patient Safety, 2, 141–150. https://doi.org/10.2147/DHPS.S7634
Slide 12 of 23
But those with few negative effects on sexual functioning include bupropion, in the studies SR version was used; mirtazapine, nefazodone, the selegiline transdermal system which is a transdermal MAOI; reboxetine, a norepinephrine reuptake inhibitor; duloxetine and desvenlafaxine which are SNRIs but they are newer ones, and vilazodone, vortioxetine, agomelatine and most recently gepirone ER which have atypical effects on neurotransmitters.
References:
- Serretti, A., & Chiesa, A. (2009). Treatment-emergent sexual dysfunction related to antidepressants: A meta-analysis. Journal of Clinical Psychopharmacology, 29(3), 259–266. https://doi.org/10.1097/JCP.0b013e3181a5233f
- Clayton, A. H., Pradko, J. F., Croft, H. A., Montano, C. B., Leadbetter, R. A., Bolden-Watson, C., Bass, K. I., Donahue, R. M., Jamerson, B. D., & Metz, A. (2002). Prevalence of sexual dysfunction among newer antidepressants. The Journal of Clinical Psychiatry, 63(4), 357–366. https://doi.org/10.4088/jcp.v63n0414
- Higgins, A., Nash, M., & Lynch, A. M. (2010). Antidepressant-associated sexual dysfunction: impact, effects, and treatment. Drug, Healthcare and Patient Safety, 2, 141–150. https://doi.org/10.2147/DHPS.S7634
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 13 of 23
I’m going to talk about post SSRI sexual dysfunction or PSSD. It was recognized by the EMA in 2019 but it has not been identified as a distinct condition by the FDA, DSM-5-TR or the ICD-11. This syndrome is based on patient reports. There are no published studies.
References:
- Nelson, C. J., Clayton, A. H., Lew-Starowicz, M., et al. (n.d.). Psychiatric disorders, psychopharmacology and sexual dysfunction. Sexual Medicine Reviews (ISSM Committee 3 publication). International Society for Sexual Medicine. https://www.issm.info/page/155
- Healy, D., & Mangin, D. (2024). Post-SSRI sexual dysfunction: barriers to quantifying incidence and prevalence. Epidemiology and Psychiatric Sciences, 33, e40. https://doi.org/10.1017/S2045796024000441
Slide 14 of 23
PSSD is described as treatment emergent sexual dysfunction persisting after SSRI, SNRI or TCA discontinuation. The proposed diagnostic criteria include enduring change in somatic, that is tactile, or erogenous, that is sexual or genital sensation, after SSRI treatment.
References:
- Healy, D., Le Noury, J., & Mangin, D. (2018). Enduring sexual dysfunction after treatment with antidepressants, 5α-reductase inhibitors and isotretinoin: 300 cases. International Journal of Risk & Safety in Medicine, 29(3–4), 125–134. https://doi.org/10.3233/JRS-180744
- Higgins, A., Nash, M., & Lynch, A. M. (2010). Antidepressant-associated sexual dysfunction: impact, effects, and treatment. Drug, Healthcare and Patient Safety, 2, 141–150. https://doi.org/10.2147/DHPS.S7634
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 15 of 23
The most common complaints include genital anesthesia or numbness, weak or pleasureless orgasmic sensations, decreased sexual drive, ejaculation difficulties and decreased vaginal lubrication. So this is pretty much pansexual dysfunction. And emotional and cognitive problems and poor quality of life are reported.
References:
- Healy, D., Le Noury, J., & Mangin, D. (2018). Enduring sexual dysfunction after treatment with antidepressants, 5α-reductase inhibitors and isotretinoin: 300 cases. International Journal of Risk & Safety in Medicine, 29(3–4), 125–134. https://doi.org/10.3233/JRS-180744
- Healy, D., Bahrick, A., Bak, M., Barbato, A., Calabrò, R. S., Chubak, B. M., Cosci, F., Csoka, A. B., D'Avanzo, B., Diviccaro, S., Giatti, S., Goldstein, I., Graf, H., Hellstrom, W. J. G., Irwig, M. S., Jannini, E. A., Janssen, P. K. C., Khera, M., Kumar, M. T., Le Noury, J., … Waraich, A. (2022). Diagnostic criteria for enduring sexual dysfunction after treatment with antidepressants, finasteride and isotretinoin. The International Journal of Risk & Safety in Medicine, 33(1), 65–76. https://doi.org/10.3233/JRS-210023
Slide 16 of 23
It’s important to differentiate these symptoms from sexual dysfunction associated with a recurrence of symptoms of the underlying condition such as anxiety or depression-related sexual dysfunction for which the antidepressant was prescribed. Also, bupropion, a known antidote for sexual dysfunction with SSRIs, was ineffective and so it suggests actually a potential alternative etiology. Men overwhelmingly predominate.
References:
- Nelson, C. J., Clayton, A. H., Lew-Starowicz, M., et al. (n.d.). Psychiatric disorders, psychopharmacology and sexual dysfunction. Sexual Medicine Reviews (ISSM Committee 3 publication). International Society for Sexual Medicine. https://www.issm.info/page/155
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 17 of 23
The incidence of PSSD is rare given the number of worldwide prescriptions for serotonin antidepressants and evaluation for underlying modifiable causes includes identification of recurrence of the underlying psychiatric disorder which requires measurement by a patient-reported outcome measure like the PHQ-9, GAD-7, etc. and also taking a sexual history to exclude other potential etiologies of sexual dysfunction.
References:
- Nelson, C. J., Clayton, A. H., Lew-Starowicz, M., et al. (n.d.). Psychiatric disorders, psychopharmacology and sexual dysfunction. Sexual Medicine Reviews (ISSM Committee 3 publication). International Society for Sexual Medicine. https://www.issm.info/page/155
- Higgins, A., Nash, M., & Lynch, A. M. (2010). Antidepressant-associated sexual dysfunction: impact, effects, and treatment. Drug, Healthcare and Patient Safety, 2, 141–150. https://doi.org/10.2147/DHPS.S7634
Slide 18 of 23
Currently, interventions mostly include management of identified medical and psychiatric causes of sexual dysfunction like smoking, substance use disorders, anxiety or depressive disorder recurrence. And potential treatment may include managing the recurrent anxiety or other psychiatric disorder with a non-SRI medication or psychotherapy.
References:
- Nelson, C. J., Clayton, A. H., Lew-Starowicz, M., et al. (n.d.). Psychiatric disorders, psychopharmacology and sexual dysfunction. Sexual Medicine Reviews (ISSM Committee 3 publication). International Society for Sexual Medicine. https://www.issm.info/page/155
- Higgins, A., Nash, M., & Lynch, A. M. (2010). Antidepressant-associated sexual dysfunction: impact, effects, and treatment. Drug, Healthcare and Patient Safety, 2, 141–150. https://doi.org/10.2147/DHPS.S7634
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 19 of 23
No prospective studies have been done because this is a rare condition and the numbers required for evaluating for this occurrence before anyone is started on an SRI is astronomical numbers. So you may hear these complaints. It’s unclear what the actual etiology is but please rule out modifiable causes or recurrence of the underlying disorder.
References:
- Nelson, C. J., Clayton, A. H., Lew-Starowicz, M., et al. (n.d.). Psychiatric disorders, psychopharmacology and sexual dysfunction. Sexual Medicine Reviews (ISSM Committee 3 publication). International Society for Sexual Medicine. https://www.issm.info/page/155
- Healy, D., & Mangin, D. (2024). Post-SSRI sexual dysfunction: barriers to quantifying incidence and prevalence. Epidemiology and Psychiatric Sciences, 33, e40. https://doi.org/10.1017/S2045796024000441
Slide 20 of 23
So our key points are: Differences in CNS fMRI imaging in men watching a non-erotic video versus an erotic video show negative effects of the SSRI paroxetine in the anterior cingulate cortex, anterior and posterior midcingulate and midbrain structures such as the nucleus accumbens and ventral striatum and on ratings of sexual functioning. In contrast, bupropion, a norepinephrine and dopamine reuptake inhibitor, was associated with enhanced brain activation in the same areas as well as in the amygdala and thalamus.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 21 of 23
Genetics play a role in sexual dysfunction assessed with the Changes in Sexual Functioning Questionnaire or CSFQ is associated with the serotonin 2A-1438 GG genotype, and the SLC6A4 promoter region for the serotonin transporter with the latter showing an eight-fold greater risk of sexual dysfunction in women with the LL genotype taking oral contraceptives.
Slide 22 of 23
A large prevalence study of sexual dysfunction with antidepressants showed variation by drug class with 70% to 80% of patients taking SSRIs, 45% of patients on SNRIs or tricyclic antidepressants, and less than 10% or similar to placebo of individuals on bupropion or agomelatine experiencing sexual dysfunction.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.