Slides and Transcript
Slide 1 of 25
Welcome to video number 7, Treatment Strategies for Managing Insomnia in Major Depressive Disorder. What are the treatment strategies for managing insomnia in patients with major depressive disorder?
Slide 2 of 25
Insomnia disorder is a common and a challenging condition to treat in patients with major depressive disorder. The treatment of insomnia should be personalized to address psychiatric, medical, sleep and lifestyle factors that may precipitate and/or perpetuate insomnia.
References:
- Chopra, A., Das, P., & Doghramji, K. (2020). Management of sleep disorders in psychiatry (1st ed.). Oxford University Press.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 3 of 25
In this section, we will discuss and evaluate the evidence for multiple treatment strategies targeting insomnia disorder comorbid with major depressive disorder. Secondly, we will review the evidence base supporting cognitive behavioral therapy or CBT-I including digital CBT-I for management of insomnia complaints in patients with major depressive disorder. Finally, advanced treatment interventions including ketamine and neuromodulation interventions such as transcranial magnetic stimulation or TMS, electroconvulsive therapy or ECT and vagal nerve stimulation or VNS may hold potential for improving insomnia outcomes in patients especially those with treatment-resistant major depression.
References:
- Manber, R., Buysse, D. J., Edinger, J., Krystal, A., Luther, J. F., Wisniewski, S. R., … & Thase, M. E. (2016). Efficacy of cognitive-behavioral therapy for insomnia combined with antidepressant pharmacotherapy in patients with comorbid depression and insomnia: A randomized controlled trial. The Journal of Clinical Psychiatry, 77(10), 2446.
Slide 4 of 25
The treatment strategies include conventional strategies used in clinical practice such as adding sedating antidepressants, non-benzodiazepine hypnotics and use of atypical antipsychotics.
References:
- Chopra, A., Das, P., & Doghramji, K. (2020). Management of sleep disorders in psychiatry (1st ed.). Oxford University Press.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 5 of 25
Insomnia may improve in parallel with other depressive symptoms in response to the standard first-line antidepressant medications such as SSRIs. However, some patients may have severe insomnia to be intolerable during the weeks required for antidepressant medications to take effect or insomnia may persist despite improvements in other depressive symptoms.
References:
- Chopra, A., Das, P., & Doghramji, K. (2020). Management of sleep disorders in psychiatry. Oxford University Press.
Slide 6 of 25
Medications including trazodone, mirtazapine and tricyclic antidepressants can be prescribed as a monotherapy or as an adjunct to first-line treatments such as SSRIs or SNRIs. These medications are used commonly in clinical practice. However, the evidence supporting the use of sedating antidepressants in treatment of insomnia in major depressive disorder is rather slim.
References:
- Chopra, A., Das, P., & Doghramji, K. (2020). Management of sleep disorders in psychiatry. Oxford University Press.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 7 of 25
The increase in slow wave sleep caused by sedating antidepressants is attributed to 5-HT2A, 2C antagonism. The clinicians are advised to consider discontinuing the sedating antidepressants to determine if insomnia has responded to the primary antidepressant treatment in order to reduce side effects and polypharmacy risks.
References:
- Chopra, A., Das, P., & Doghramji, K. (2020). Management of sleep disorders in psychiatry (1st ed.). Oxford University Press.
Slide 8 of 25
In terms of sedating antidepressants, trazodone which acts on 5-HT2 and alpha-1 receptors is commonly used for treatment of insomnia in patients with major depressive disorder. The usual dosing for insomnia with the use of trazodone is 50 to 150 mg before bedtime. Use of trazodone has been associated with decreased wake after sleep onset, increased total sleep time and increased stage N3 sleep.
References:
- Chopra, A., Das, P., & Doghramji, K. (2020). Management of sleep disorders in psychiatry (1st ed.). Oxford University Press.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 9 of 25
Mirtazapine which acts primarily on histaminergic receptors is used for treatment of insomnia at dosages 7.5 to 15 mg before bedtime. It has been associated with decreased sleep onset latency, increased total sleep time and increased stage N3 sleep.
References:
- Chopra, A., Das, P., & Doghramji, K. (2020). Management of sleep disorders in psychiatry (1st ed.). Oxford University Press.
Slide 10 of 25
Atypical antipsychotics are increasingly prescribed for the management of major depressive disorder and medications including quetiapine, olanzapine in combination with fluoxetine, aripiprazole, brexpiprazole and cariprazine have been FDA approved as adjunct treatments for major depression.
References:
- Chopra, A., Das, P., & Doghramji, K. (2020). Management of sleep disorders in psychiatry (1st ed.). Oxford University Press.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 11 of 25
The role of atypical antipsychotics in treating insomnia complaints in patients with major depressive disorder has been investigated in a few studies. Quetiapine extended release dosage between 50 to 300 mg has been examined for efficacy in improving sleep outcomes in patients with major depressive disorder. Both objective and subjective improvements in sleep quality have been reported for quetiapine extended release both as an adjunct and monotherapy for major depressive disorder.
References:
- Chopra, A., Das, P., & Doghramji, K. (2020). Management of sleep disorders in psychiatry (1st ed.). Oxford University Press.
Slide 12 of 25
Adjunct treatment with olanzapine has been associated with improvements in sleep onset latency, sleep efficiency and total sleep time in patients with major depressive disorder based on polysomnography findings.
References:
- Chopra, A., Das, P., & Doghramji, K. (2020). Management of sleep disorders in psychiatry (1st ed.). Oxford University Press.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 13 of 25
When prescribing atypical antipsychotics, clinicians are advised to monitor for side effects such as daytime somnolence, weight gain, extrapyramidal side effects, metabolic side effects and risk for tardive dyskinesia.
References:
- Chopra, A., Das, P., & Doghramji, K. (2020). Management of sleep disorders in psychiatry (1st ed.). Oxford University Press.
Slide 14 of 25
Concern for sleep walking and sleep-related eating behaviors associated with atypical antipsychotic use has been reported in the literature. Clinicians are advised to screen for sleep-related eating in patients with atypical antipsychotics presenting with symptoms of weight gain.
References:
- Chopra, A., Das, P., & Doghramji, K. (2020). Management of sleep disorders in psychiatry (1st ed.). Oxford University Press.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 15 of 25
In one study using the combination of fluoxetine and eszopiclone at a dose of 3 mg nightly, the authors found improvements in both subjective sleep quality and objective sleep parameters such as total sleep time, wake after sleep onset time and sleep efficiency with the use of fluoxetine and eszopiclone combination as compared to fluoxetine and placebo. Additionally, patients on this drug combination had a faster onset of antidepressant response and a greater magnitude of antidepressant effect as compared to fluoxetine and placebo combination.
References:
- Fava, M., McCall, W. V., Krystal, A., Wessel, T., Rubens, R., Caron, J., … & Roth, T. (2006). Eszopiclone co-administered with fluoxetine in patients with insomnia coexisting with major depressive disorder. Biological Psychiatry, 59(11), 1052-1060.
Slide 16 of 25
Two other studies using zolpidem 10 mg immediate-release formulation and zolpidem 12.5 mg extended-release formulation in addition to SSRIs showed similar effects in terms of sleep outcomes but without augmentation of antidepressant effects.
References:
- Chopra, A., Das, P., & Doghramji, K. (2020). Management of sleep disorders in psychiatry (1st ed.). Oxford University Press.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 17 of 25
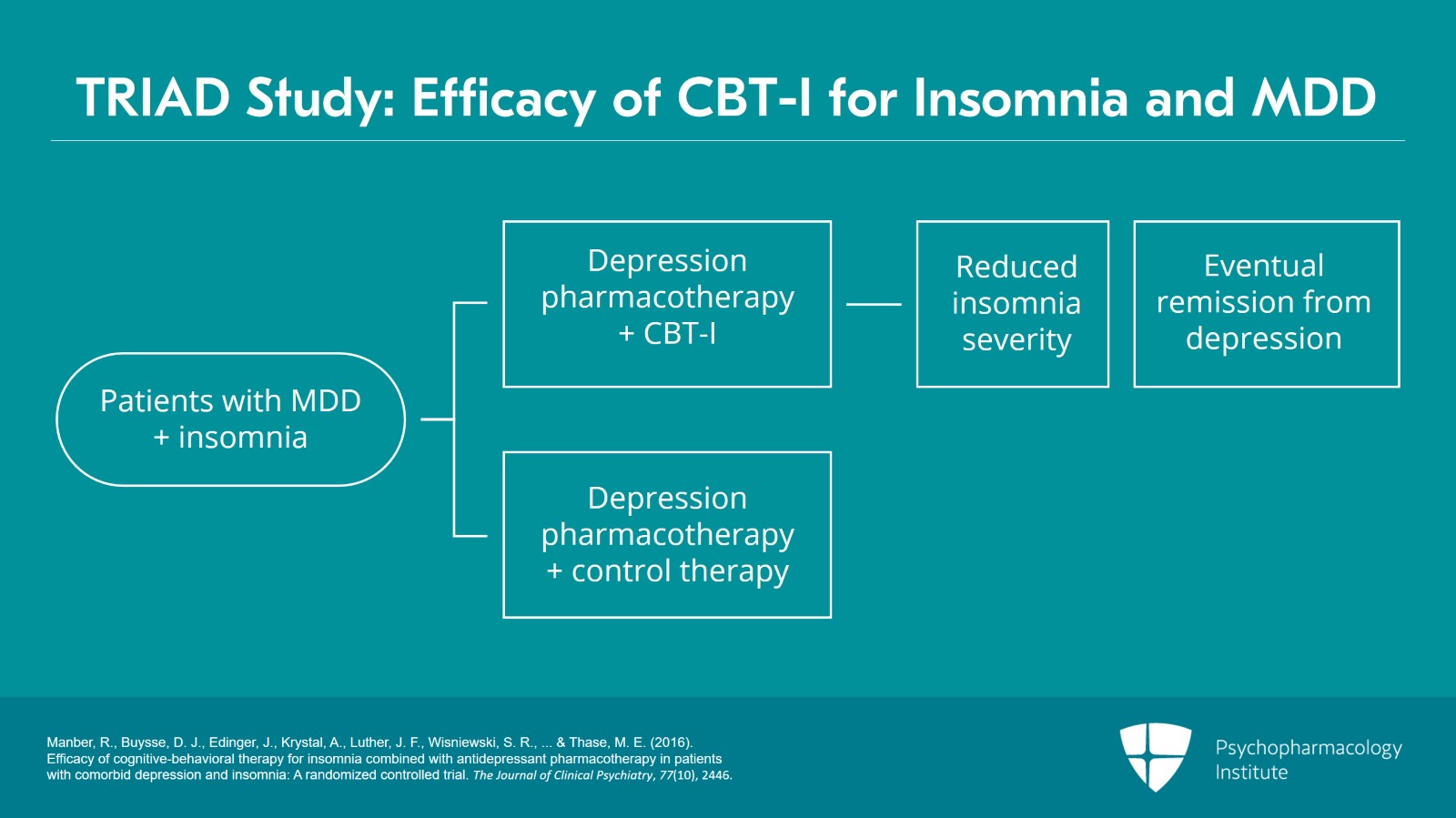
The efficacy of CBT-I for insomnia has been evaluated in patients with major depressive disorder taking standard antidepressant treatments in multiple studies. In a 16-week, three-site randomized controlled trial named as Treatment of Insomnia and Depression Study or TRIAD Study, 150 adult participants with major depressive disorder and insomnia were randomly assigned to depression pharmacotherapy plus seven sessions of either CBT-I or control therapy for insomnia that included sleep education. The authors noted that CBT-I was superior to control intervention in significantly reducing insomnia severity but not depression. However, improvements in insomnia at six weeks mediated eventual remission from depression as an early change in insomnia severity predicted depression remission in the CBT-I group but not the control group.
References:
- Manber, R., Buysse, D. J., Edinger, J., Krystal, A., Luther, J. F., Wisniewski, S. R., … & Thase, M. E. (2016). Efficacy of cognitive-behavioral therapy for insomnia combined with antidepressant pharmacotherapy in patients with comorbid depression and insomnia: A randomized controlled trial. The Journal of clinical psychiatry, 77(10), 2446.
Slide 18 of 25
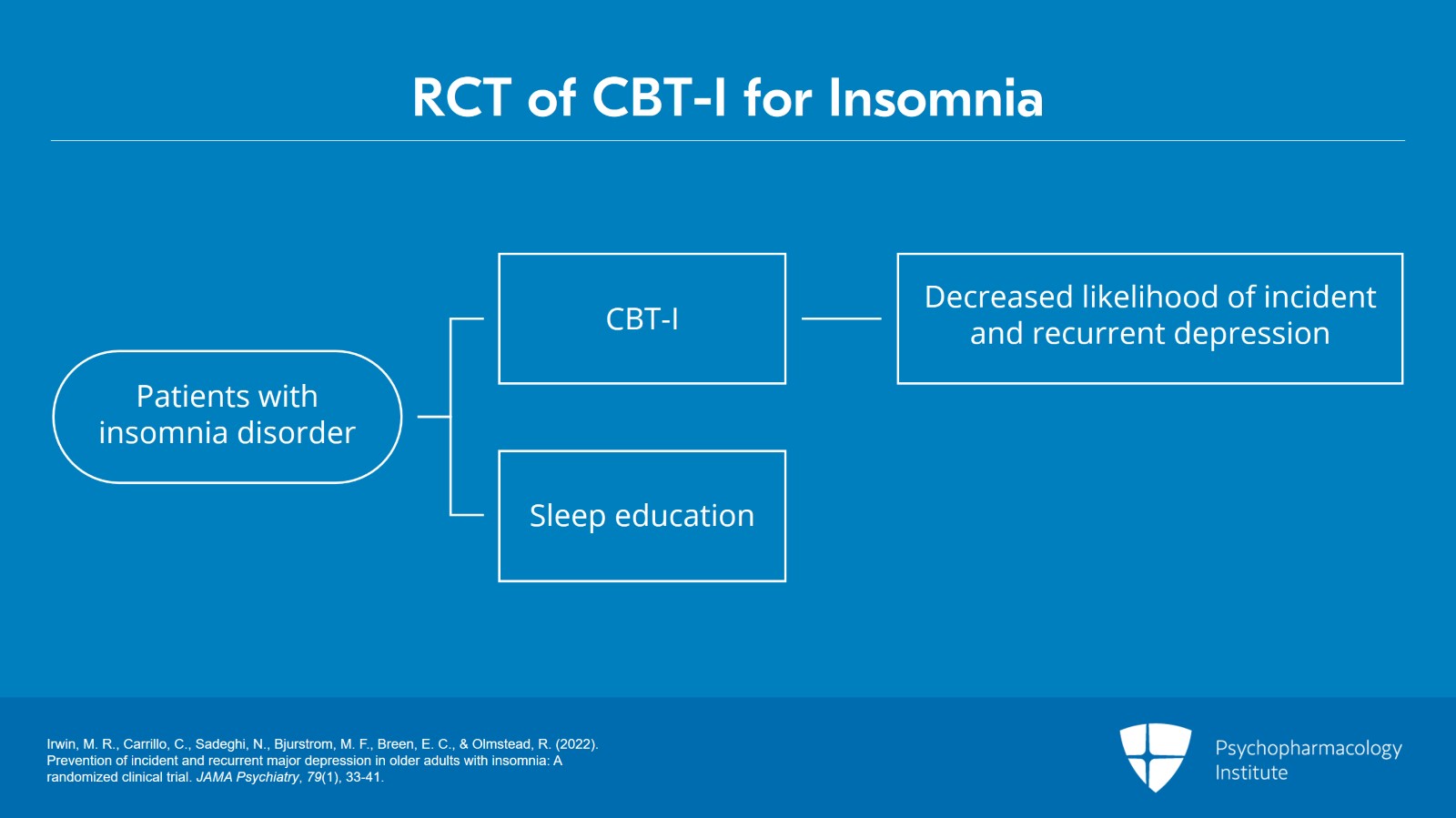
In another randomized clinical trial of 291 adult patients who were 60 years or older and had insomnia disorder, two months of cognitive behavioral therapy for insomnia or CBT-I resulted in a decreased likelihood of incident and recurrent depression during 36 months of follow-up compared with sleep education therapy. Sustained insomnia remission in adults undergoing CBT-I resulted in decreased likelihood of developing depression versus no insomnia remission in adults receiving sleep education in this study.
References:
- Irwin, M. R., Carrillo, C., Sadeghi, N., Bjurstrom, M. F., Breen, E. C., & Olmstead, R. (2022). Prevention of incident and recurrent major depression in older adults with insomnia: A randomized clinical trial. JAMA Psychiatry, 79(1), 33-41.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 19 of 25
Digital CBT-I has been approved by FDA for treatment of insomnia disorder since 2020. The effect of digital CBT-I has been examined in alleviating insomnia and mood symptoms in different studies.
References:
- Cheng, P., Kalmbach, D. A., Tallent, G., Joseph, C. L., Espie, C. A., & Drake, C. L. (2019). Depression prevention via digital cognitive behavioral therapy for insomnia: A randomized controlled trial. Sleep, 42(10), zsz150.
Slide 20 of 25
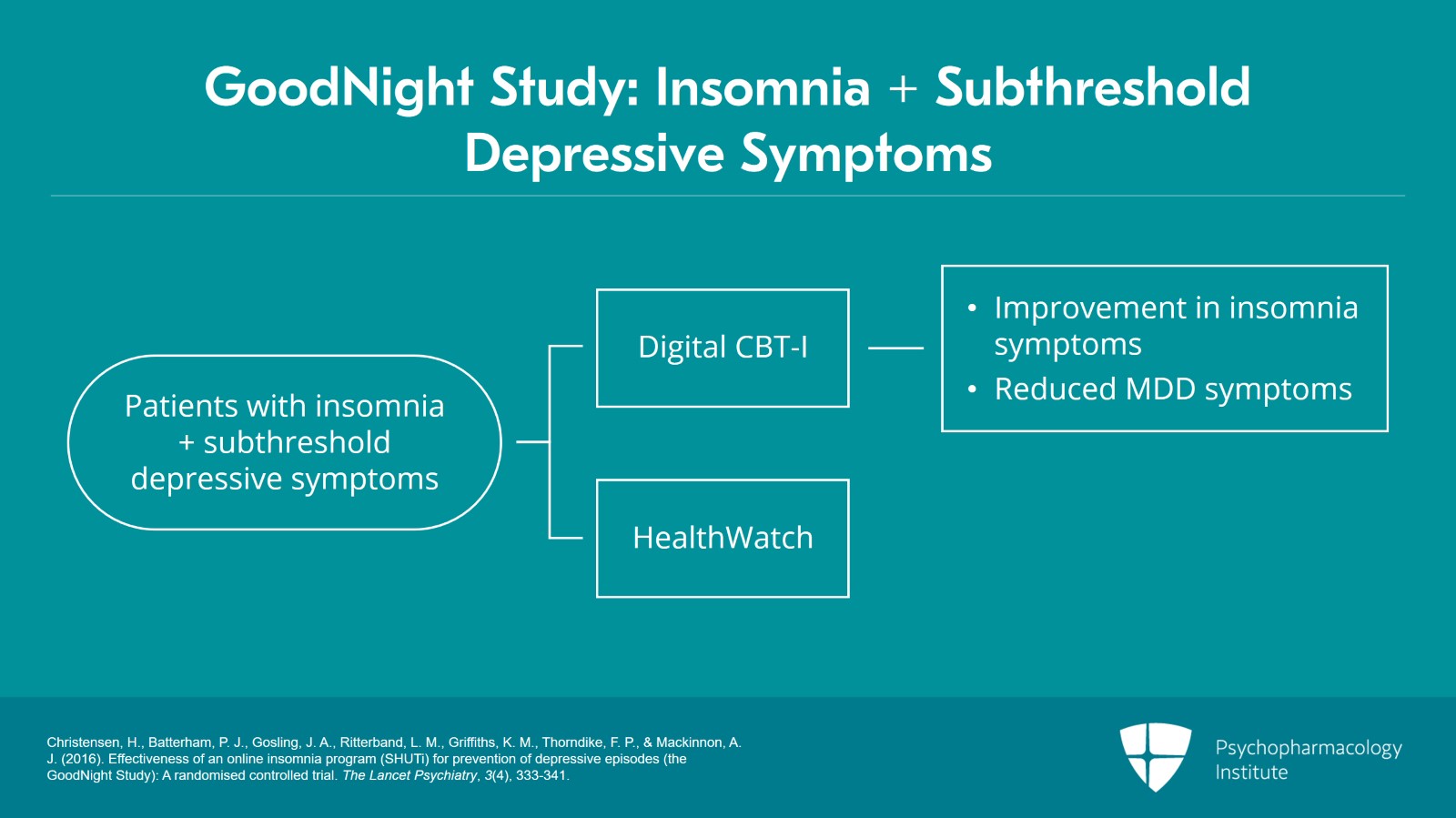
The GoodNight Study included a large sample size of 1149 adult patients with insomnia and subthreshold depression symptoms who were randomized to digital CBT-I and HealthWatch which is an internet-based placebo treatment. The authors reported that digital CBT-I significantly improved insomnia symptoms and reduced depressive symptoms at six weeks and six months. However, digital CBT-I did not significantly reduce the number of participants with major depressive disorder compared to placebo at follow-up.
References:
- Christensen, H., Batterham, P. J., Gosling, J. A., Ritterband, L. M., Griffiths, K. M., Thorndike, F. P., & Mackinnon, A. J. (2016). Effectiveness of an online insomnia program (SHUTi) for prevention of depressive episodes (the GoodNight Study): A randomised controlled trial. The Lancet Psychiatry, 3(4), 333-341.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 21 of 25
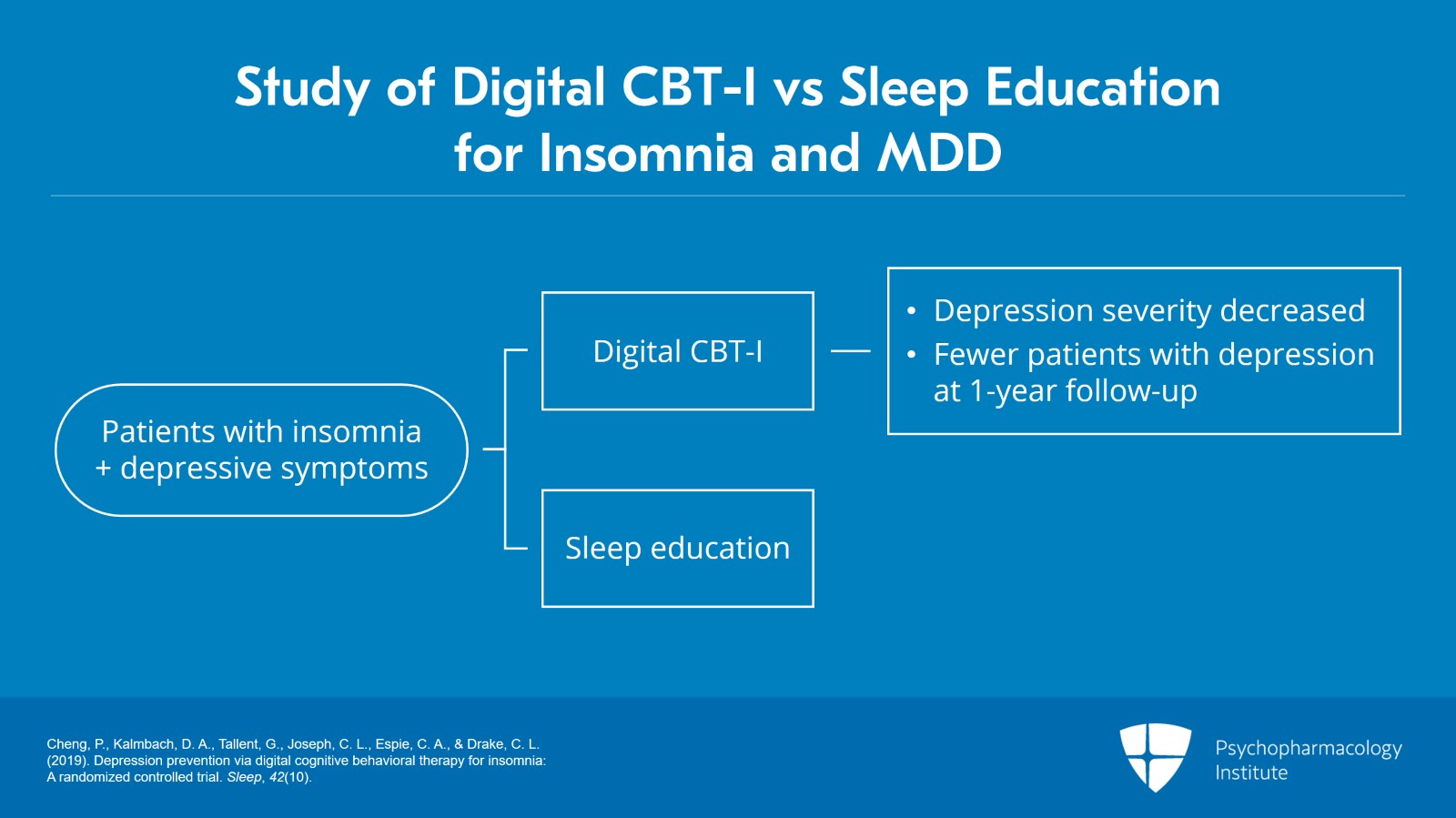
In another digital CBT-I study, the authors examined the efficacy of digital CBT-I in terms of depression prevention in subjects with insomnia. 658 adults with insomnia disorder approximately half of whom had depressive symptoms rated as moderate or worse at baseline were randomized to digital CBT-I or online sleep education. At one-year follow-up, depression severity continued to be significantly lower in the digital CBT-I group relative to control condition. Also, the number of individuals who reported no depression at one-year follow-up was 51% higher in the digital CBT-I condition as compared to the control intervention. Additionally, in those subjects with minimal to no depression at baseline, the incident rate of moderate to severe depression at one-year followup was reduced by half in the digital CBT-I intervention relative to the control intervention.
References:
- Cheng, P., Kalmbach, D. A., Tallent, G., Joseph, C. L., Espie, C. A., & Drake, C. L. (2019). Depression prevention via digital cognitive behavioral therapy for insomnia: A randomized controlled trial. Sleep, 42(10).
Slide 22 of 25
Insomnia is a clinical risk factor for suicide independent of depression severity. There's very limited data examining the effects of insomnia treatments on suicidal ideations in patients with insomnia disorder and major depression.
References:
- McCall, W. V., Benca, R. M., Rosenquist, P. B., Youssef, N. A., McCloud, L., Newman, J. C., … & Krystal, A. D. (2019). Reducing suicidal ideation through insomnia treatment (REST-IT): a randomized clinical trial. American Journal of Psychiatry, 176(11), 957-965.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 23 of 25
Reducing suicidal ideations through insomnia treatment or REST-IT Study examined the effects of extended-release zolpidem versus placebo with open-label SSRI use in patients with major depression, insomnia and co-occurring SI in an eight-week, three-site double-blind RCT with 103 adult participants. Suicidal ideation was the main outcome and it was measured by using scales such as Scale for Suicide Ideation and Columbia-Suicide Severity Rating Scale. Insomnia severity was assessed using Insomnia Severity Index. The authors reported that co-prescription of zolpidem ER 6.25 to 12.5 mg nightly with SSRI reduced SI particularly in the patients with more severe insomnia. No deaths or suicide attempts were reported in this study.
References:
- McCall, W. V., Benca, R. M., Rosenquist, P. B., Youssef, N. A., McCloud, L., Newman, J. C., … & Krystal, A. D. (2019). Reducing suicidal ideation through insomnia treatment (REST-IT): a randomized clinical trial. American Journal of Psychiatry, 176(11), 957-965.
Slide 24 of 25
Key points. Different treatment strategies including sedating antidepressants, non-benzodiazepine hypnotics and atypical antipsychotics are used for treatment of insomnia disorder in patients with major depressive disorder. CBT-I has been shown to improve insomnia in patients with major depressive disorder and it may likely have antidepressant effects. Digital CBT-I is an effective intervention for improving insomnia disorder symptoms and it has been shown to significantly reduce the incidence of depression during one-year followup as compared to the control interventions.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.