Slides and Transcript
Slide 2 of 14
So note that with the second-generation antipsychotics, I consider them to be third-line augmentation only. I will often see patients who are started on second-generation antipsychotics as they are started on SSRIs. Various reasons are given for that by the prescribing clinicians, and I will tell you that there is no evidence that second-generation antipsychotics have any benefit at all early on in OCD treatment. So it’s not recommended.
References:
- Veale, D., Miles, S., Smallcombe, N., Ghezai, H., Goldacre, B., & Hodsoll, J. (2014). Atypical antipsychotic augmentation in SSRI treatment refractory obsessive–compulsive disorder: A systematic review and meta-analysis. BMC Psychiatry, 14, 317. https://doi.org/10.1186/s12888-014-0317-5
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 3 of 14
The response for a second-generation antipsychotic for OCD augmentation is usually seen in four to six weeks. I give my patients a two-month trial, and if they don’t get significant improvement, I pull the second-generation antipsychotic. Note that if patients have schizotypal-type symptoms, so odd beliefs that are associated with the OCD or if they have delusional level of insight, antipsychotics are not recommended.
References:
- Veale, D., Miles, S., Smallcombe, N., Ghezai, H., Goldacre, B., & Hodsoll, J. (2014). Atypical antipsychotic augmentation in SSRI treatment refractory obsessive–compulsive disorder: A systematic review and meta-analysis. BMC Psychiatry, 14, 317. https://doi.org/10.1186/s12888-014-0317-5
- Borue, X., Sharma, M., & Hudak, R. (2015). Biological treatments for obsessive-compulsive and related disorders. Journal of Obsessive-Compulsive and Related Disorders, 6, 7-26. https://doi.org/10.1016/j.jocrd.2015.03.003
Slide 4 of 14
With second-generation, notice that patients with tics may have an improved response over other OCD patients, but there are no specific characteristics of the OCD itself that have been identified that relate to response of second-generation antipsychotics. So once you diagnose someone with OCD, it doesn’t matter what type of OCD symptoms that they have, we don’t know of any medication treatment that’s tailored to fit actual OCD subtypes or symptoms.
References:
- Bloch, M. H., Landeros-Weisenberger, A., Kelmendi, B., Coric, V., Bracken, M. B., & Leckman, J. F. (2006). A systematic review: Antipsychotic augmentation with treatment refractory obsessive-compulsive disorder. Molecular Psychiatry, 11(7), 622–632. https://doi.org/10.1038/sj.mp.4001823
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 5 of 14
Now, be aware that second-generation antipsychotics are not a homogenous group of medication. You just don’t prescribe any second-generation antipsychotic for OCD willy-nilly. These are very different groups of medications. And the doses we use for the SGAs are much less than the one we use for bipolar disorder or psychosis.
References:
- Veale, D., Miles, S., Smallcombe, N., Ghezai, H., Goldacre, B., & Hodsoll, J. (2014). Atypical antipsychotic augmentation in SSRI treatment refractory obsessive–compulsive disorder: A systematic review and meta-analysis. BMC Psychiatry, 14, 317. https://doi.org/10.1186/s12888-014-0317-5
- Bloch, M. H., Landeros-Weisenberger, A., Kelmendi, B., Coric, V., Bracken, M. B., & Leckman, J. F. (2006). A systematic review: Antipsychotic augmentation with treatment refractory obsessive-compulsive disorder. Molecular Psychiatry, 11(7), 622–632. https://doi.org/10.1038/sj.mp.4001823
Slide 6 of 14
Now, I note that the second-generation antipsychotics may worsen OCD as well as augment. There had been numerous case reports of SGAs worsening OCD. So you do have to be careful with that. It has been reported with clozapine, in particular clozapine quite often makes OCD much worse. Olanzapine, risperidone, and quetiapine have also been reported to have worsening of OCD symptoms as well as augmenting OCD symptoms. They are less studied in children.
References:
- Veale, D., Miles, S., Smallcombe, N., Ghezai, H., Goldacre, B., & Hodsoll, J. (2014). Atypical antipsychotic augmentation in SSRI treatment refractory obsessive–compulsive disorder: A systematic review and meta-analysis. BMC Psychiatry, 14, 317. https://doi.org/10.1186/s12888-014-0317-5
- Bleakley, S., Brown, D., & Taylor, D. (2011). Does clozapine cause or worsen obsessive compulsive symptoms? An analysis and literature review. Therapeutic Advances in Psychopharmacology, 1(6), 181-188. https://doi.org/10.1177/2045125311425971
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 7 of 14
And note that if you do have someone on a second-generation antipsychotic, they require biannual or yearly blood sugar, lipid profile and AIMS test. So you need to do the monitoring appropriately with people on second-generation antipsychotics.
References:
- Veale, D., Miles, S., Smallcombe, N., Ghezai, H., Goldacre, B., & Hodsoll, J. (2014). Atypical antipsychotic augmentation in SSRI treatment refractory obsessive–compulsive disorder: A systematic review and meta-analysis. BMC Psychiatry, 14, 317. https://doi.org/10.1186/s12888-014-0317-5
- Bloch, M. H., Landeros-Weisenberger, A., Kelmendi, B., Coric, V., Bracken, M. B., & Leckman, J. F. (2006). A systematic review: Antipsychotic augmentation with treatment refractory obsessive-compulsive disorder. Molecular Psychiatry, 11(7), 622–632. https://doi.org/10.1038/sj.mp.4001823
Slide 8 of 14
So in the order of recommendation, I typically recommend aripiprazole as my top line second-generation antipsychotic. It did show to work with a double-blind randomized controlled trial. The response rates were similar to risperidone. While it doesn’t have quite as much evidence of risperidone, it does have less side effects. The usual dose is about 2 to 15 mg, and note that it’s the only one of the recommended antipsychotics that has not been shown to worsen OCD symptoms.
References:
- Dold, M., Aigner, M., Lanzenberger, R., & Kasper, S. (2015). Antipsychotic augmentation of serotonin reuptake inhibitors in treatment-resistant obsessive-compulsive disorder: An update meta-analysis of double-blind, randomized, placebo-controlled trials. International Journal of Neuropsychopharmacology, 18(9), pyv047. https://doi.org/10.1093/ijnp/pyv047
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 9 of 14
Risperidone is the one SGA that has the most evidence as an augmenter. It has a double-blind randomized controlled trial. And the usual dose is 0.5 to 2 mg a day.
References:
- Dold, M., Aigner, M., Lanzenberger, R., & Kasper, S. (2015). Antipsychotic augmentation of serotonin reuptake inhibitors in treatment-resistant obsessive-compulsive disorder: An update meta-analysis of double-blind, randomized, placebo-controlled trials. International Journal of Neuropsychopharmacology, 18(9), pyv047. https://doi.org/10.1093/ijnp/pyv047
Slide 10 of 14
Olanzapine has some double-blind, randomized controlled trials, not nearly as much as the others. It may also worsen OCD and so you need to be very careful with olanzapine. Usual dose is 2.5 to 15 mg a day.
References:
- Dold, M., Aigner, M., Lanzenberger, R., & Kasper, S. (2015). Antipsychotic augmentation of serotonin reuptake inhibitors in treatment-resistant obsessive-compulsive disorder: An update meta-analysis of double-blind, randomized, placebo-controlled trials. International Journal of Neuropsychopharmacology, 18(9), pyv047. https://doi.org/10.1093/ijnp/pyv047
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 11 of 14
Quetiapine seems to have less data than the others, and its data tend to be both positive and negative. Usually low dose at 50 to 200 mg daily. Now, the other second-generation antipsychotics have very little data. Therefore, I do not recommend any of the other second-generation antipsychotics.
References:
- Dold, M., Aigner, M., Lanzenberger, R., & Kasper, S. (2015). Antipsychotic augmentation of serotonin reuptake inhibitors in treatment-resistant obsessive-compulsive disorder: An update meta-analysis of double-blind, randomized, placebo-controlled trials. International Journal of Neuropsychopharmacology, 18(9), pyv047. https://doi.org/10.1093/ijnp/pyv047
Slide 12 of 14
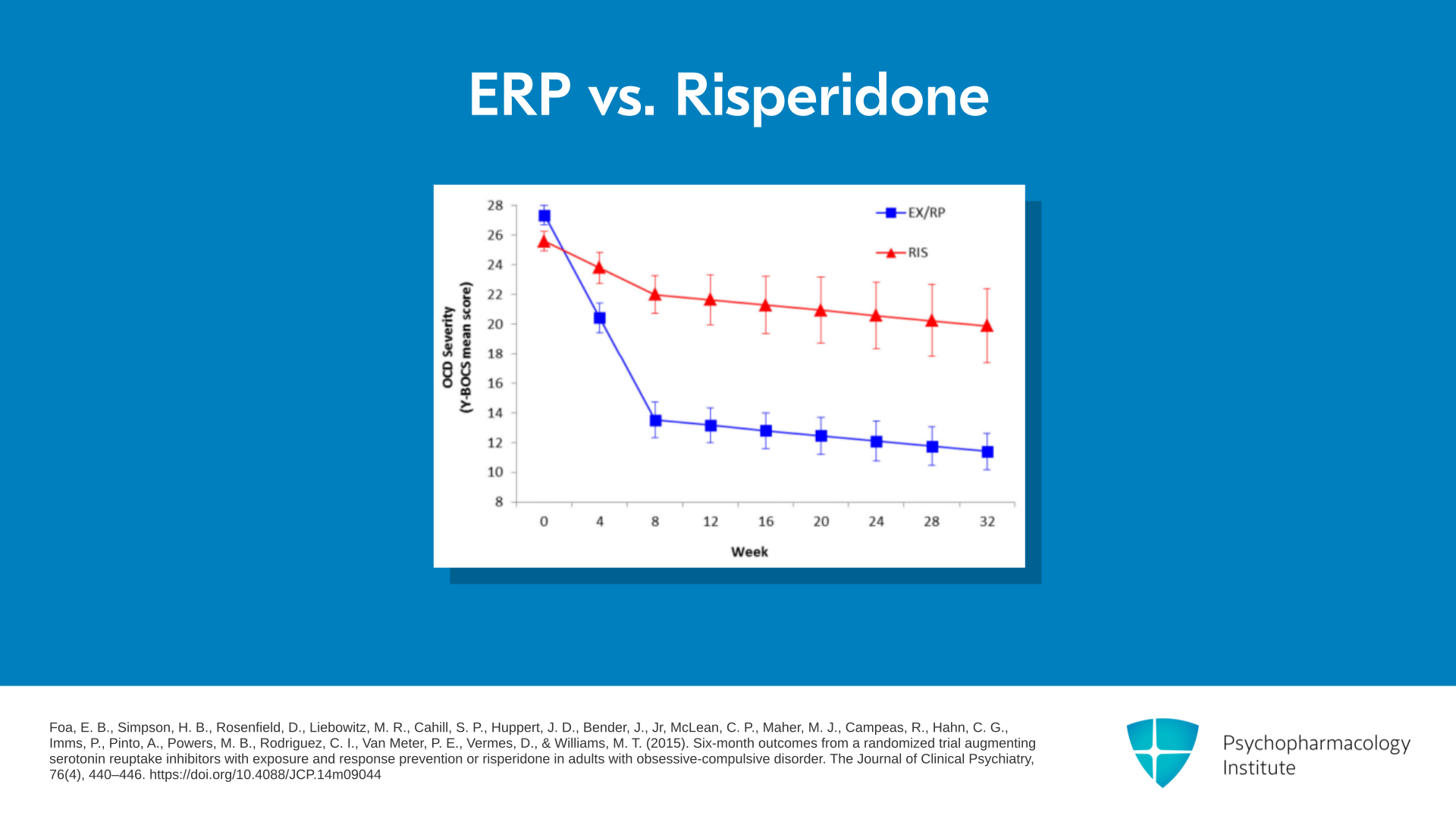
And see this graph here. What they did was that they took two groups of patients who were considered treatment-resistant OCD. They gave one ERP; they gave the second risperidone. And they found out that the response to risperidone was minimal. The response to adding ERP was pretty robust. So the take-home point from this is that appropriate and expertly performed ERP is more powerful even than risperidone augmentation. So again, always ensure that your patients are in appropriate ERP treatment. And ERP augmentation is going to be much more powerful than any other medication augmentation that we can do.
References:
- Foa, E. B., Simpson, H. B., Rosenfield, D., Liebowitz, M. R., Cahill, S. P., Huppert, J. D., Bender, J., Jr, McLean, C. P., Maher, M. J., Campeas, R., Hahn, C. G., Imms, P., Pinto, A., Powers, M. B., Rodriguez, C. I., Van Meter, P. E., Vermes, D., & Williams, M. T. (2015). Six-month outcomes from a randomized trial augmenting serotonin reuptake inhibitors with exposure and response prevention or risperidone in adults with obsessive-compulsive disorder. The Journal of Clinical Psychiatry, 76(4), 440–446. https://doi.org/10.4088/JCP.14m09044
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 13 of 14
So the key points for this. Second-generation antipsychotics are generally considered a third- or fourth-line augmentation strategy when weighing risks and benefits. Only four second generation antipsychotics have been studied enough to recommend – risperidone, aripiprazole, olanzapine and quetiapine.
Slide 14 of 14
All of these medications have been reported to exacerbate OCD as well and clozapine does in particular can exacerbate it, with the exception of aripiprazole. Second-generation antipsychotics require close monitoring and despite their efficacy as augmentation, they may even be less effective than just simply behavioral therapy.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.