Slides and Transcript
Slide 1 of 20
We've been talking in terms of ambivalence, you know. As I said, the patients may be ambivalent about caregiving, and so, I think the fourth principle of psychodynamic psychopharmacology is to foster the alliance and attend to negative transferences that lead to treatment resistance to medications.
Slide 2 of 20
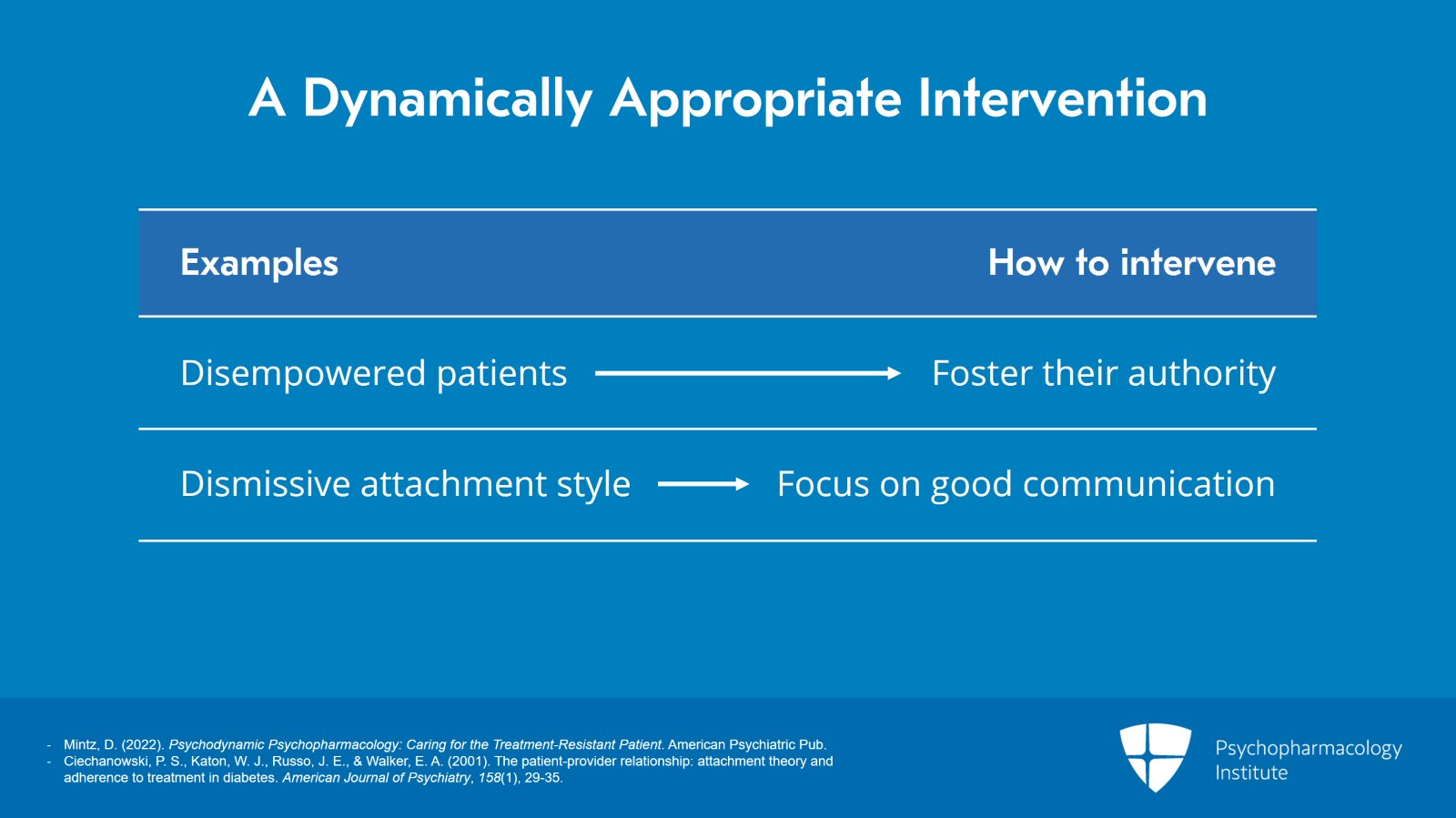
Some of the things we may want to do is, once we understand the patient's dynamics: shape our interventions in a way that does not crash into the dynamics. So, for patients who have been disempowered be especially mindful of fostering their authority. We know, for example, that patients with a dismissive attachment style tend to have worse adherence and worse outcomes, but we also know that good communication erases that effect. So, if you identified you have a patient with a dismissive attachment style, you're going to focus especially on good communication with that patient.
References:
- Mintz, D. (2022). Psychodynamic Psychopharmacology: Caring for the Treatment-Resistant Patient. American Psychiatric Pub.
- Ciechanowski, P. S., Katon, W. J., Russo, J. E., & Walker, E. A. (2001). The patient-provider relationship: attachment theory and adherence to treatment in diabetes. American Journal of Psychiatry, 158(1), 29-35.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 3 of 20
We may also want to think about increasing the dose at times, not of the drug but of the doctor, because that is a simple intervention that, you know, you can say that the patient would like to see you a little bit more often while we're doing these changes. And, when you have a sense that there are negative transferences at play, sometimes that is a simple intervention that can give you space to work that out and to change something about the way the patient feels that you're invested in them.
References:
- Mintz, D. (2022). Psychodynamic Psychopharmacology: Caring for the Treatment-Resistant Patient. American Psychiatric Pub.
Slide 4 of 20
You may also do more intentionally interpretative psychodynamic interventions by helping patients anticipate sources of resistance, aligning with the patient's healthier aspects and interpreting, in ways that you're mindful though don't interfere with the interpretative work of a psychotherapist, if they have one, attending to roles and boundaries and keeping those interpretations limited simply to the patient's use of medications.
References:
- Mintz, D. (2022). Psychodynamic Psychopharmacology: Caring for the Treatment-Resistant Patient. American Psychiatric Pub.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 5 of 20
Another principle of psychodynamic psychopharmacology is identifying and containing countertransference, acting out. Elvin Semrad, who was a legendary psychotherapy teacher in Boston and the teacher of my teachers, described the doctor-patient encounter as an encounter between a big mess and an even bigger mess. And I think it's important for us to recognize that the patient is not the only person with a capacity for irrationality in the doctor-patient relationship, and that the patient is not the only person in that room that has an unconscious.
References:
- Rako, S., & Mazer, M. (1980). Semrad: The Heart of a Therapist New York: Jason Aronson.
Slide 6 of 20
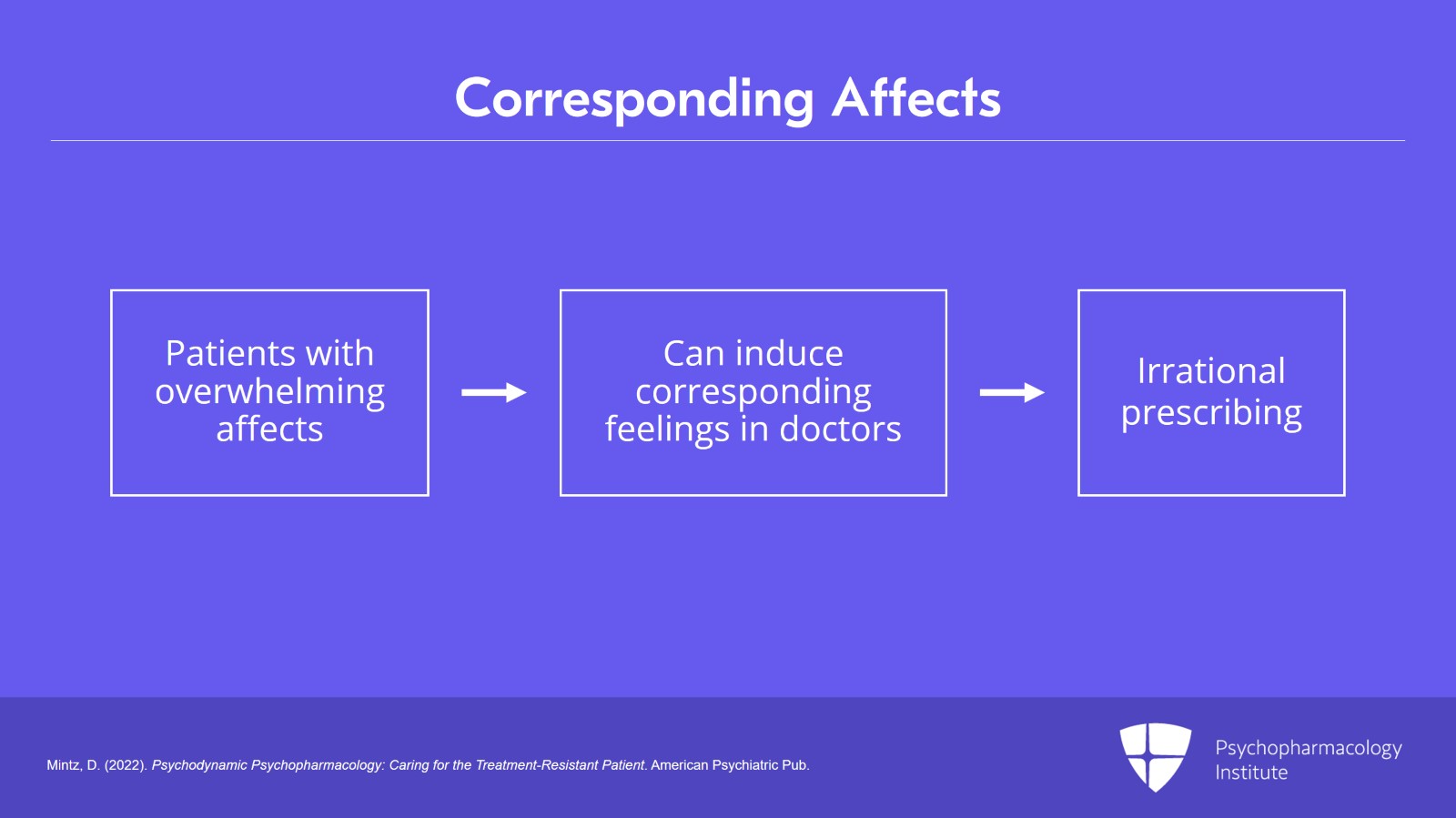
And patients who are struggling with overwhelming affects very often induce corresponding affects in others, right? So, the patients who are feeling angry can make us angry. The patients who feel helpless and hopeless can induce corresponding feelings of helplessness and hopelessness in us. And, at times, we can then prescribe in efforts not to address the patient's anxiety but to address our own, and this can lead to irrational prescribing.
References:
- Mintz, D. (2022). Psychodynamic Psychopharmacology: Caring for the Treatment-Resistant Patient. American Psychiatric Pub.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 7 of 20
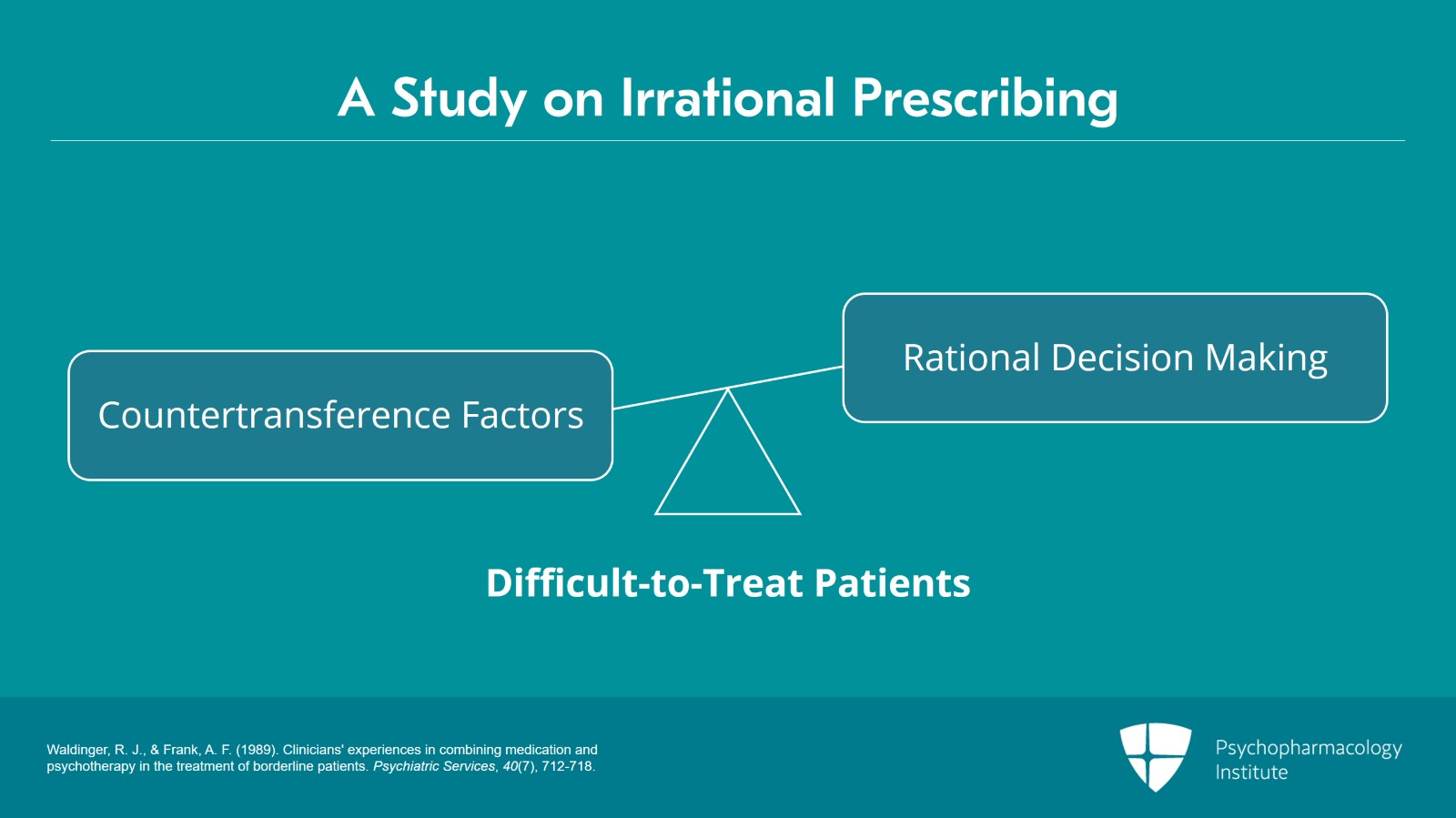
There is some research on this. Waldinger and Frank found that for difficult to treat patients, the cluster B range, countertransference factors in their analysis seem to outweigh rational decision making in the prescription of medications. So, there were often like complex, difficult to bear feelings stirred up in the doctor that started guiding treatment decisions.
References:
- Waldinger, R. J., & Frank, A. F. (1989). Clinicians' experiences in combining medication and psychotherapy in the treatment of borderline patients. Psychiatric Services, 40(7), 712-718.
Slide 8 of 20
Now, the first thing we want to do in our prescribing is to contain impulsivity, but not of the patient but of us. You know, you'd like to really step back and think. One thing that's obviously very helpful with that is consultation with colleagues when you have difficult-to-treat patients. Another thing that you can do is a dynamic formulation, and I write one of these on every patient that I see with, who has a history of treatment resistance as they come in.
References:
- Mintz, D. (2022). Psychodynamic Psychopharmacology: Caring for the Treatment-Resistant Patient. American Psychiatric Pub.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 9 of 20
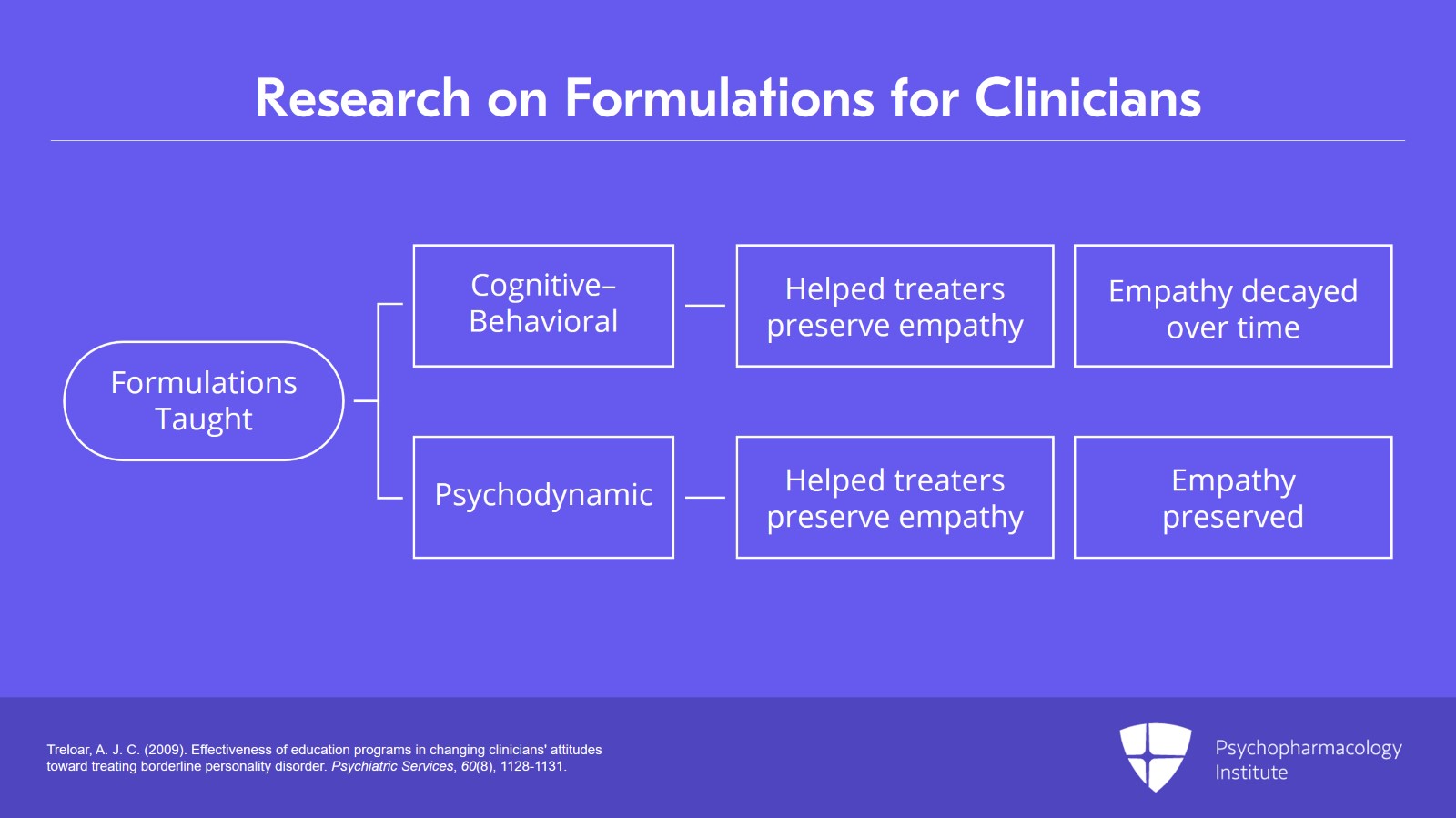
According to research by Treloar, who is a CBT clinician, they taught both cognitive-behavioral or psychodynamic formulations to frontline clinicians working in ERs with kind of repeat self-mutilators, and having a formulation helped those treaters to preserve a feeling of empathy, though, in that research, it seemed that for people who learned the cognitive behavioral formulation that feeling of empathy decayed over time, so that by six months it had decayed to non-significance. But people who had learned a psychodynamic formulation to help them understand chronic self-mutilation had preserved empathy over time. So, if we can develop a formulation about our patients, it can help us to manage our countertransference.
References:
- Treloar, A. J. C. (2009). Effectiveness of education programs in changing clinicians' attitudes toward treating borderline personality disorder. Psychiatric Services, 60(8), 1128-1131.
Slide 10 of 20
Now, in terms of this, you know, we're talking about ways that patients can fill us with things, it's not uncommon for them to present in crisis and it can be difficult to avoid making changes to medications even though medication changes are unlikely to address the underlying problem. So, what non-pharmacologic intervention should we offer patients?
References:
- Mintz, D. (2022). Psychodynamic Psychopharmacology: Caring for the Treatment-Resistant Patient. American Psychiatric Pub.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 11 of 20
Most often the crises are not ones that medications will typically address, medically at least, in a meaningful way as, given that they're desperate responses to a kind of psychosocial stressor, in a moment that's going to pass. And, when we prescribe, medications can be helpful, but more often they function more like placebos, which satisfy either the doctor's or the patient's feeling that something needs to be done. And the starting place here would be recognizing that the doctor is also having a hard time managing their own feelings and it's not the patient who is struggling with overwhelm.
References:
- Mintz, D. (2022). Psychodynamic Psychopharmacology: Caring for the Treatment-Resistant Patient. American Psychiatric Pub.
Slide 12 of 20
There are some other things I think we can do, especially before the crisis. We want to educate the patient about the actual limits of medications, some of the ways that they can become permanent solutions to temporary problems, especially in our kinds of patients who come in to us already on a raft of medications that seems kind of irrational in the beginning. We may want to explore whether the patient's distress is a problem of illness or a problem of living, is it really about depression, or is it that they have a maladaptive response to real stressors in the world, and we need to help them actually develop a better response to those real stressors or injustices that they're facing?
References:
- Mintz, D. (2022). Psychodynamic Psychopharmacology: Caring for the Treatment-Resistant Patient. American Psychiatric Pub.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 13 of 20
At times, we may want to prescribe but with an explanation that we believe the act of prescribing is probably more impactful than the actual medication so, instead of them just feeling abandoned when we don't prescribe, we're enculturating them into a way of thinking about medications that is more complex and that we're starting to teach them that medications have psychological effects as much or more than they have biomedical effects.
References:
- Mintz, D. (2022). Psychodynamic Psychopharmacology: Caring for the Treatment-Resistant Patient. American Psychiatric Pub.
Slide 14 of 20
Of course, we want to engage the patient empathically around, that our empathy is as likely to be containing as any medication. And, at times, if you're empathic enough, it substitutes for increasing medications or increased frequency in psychiatric visits. And in those situations, we want to be mindful to empower the patients as well. We're going to give them choices such as "you could try these coping skills or you could try medications“, and that act of empowerment puts them in a better position to think more clearly.
References:
- Mintz, D. (2022). Psychodynamic Psychopharmacology: Caring for the Treatment-Resistant Patient. American Psychiatric Pub.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 15 of 20
You might add when you're talking to those patients that learning to use coping skills is likely to have more lasting effects than an increase in medications. You could say like: "I think maybe you should go with the coping skills, but if those fail, then you have a backup and just let me know when we'll go with the medications." So, different strategies for trying to slow that down.
References:
- Mintz, D. (2022). Psychodynamic Psychopharmacology: Caring for the Treatment-Resistant Patient. American Psychiatric Pub.
Slide 16 of 20
And, as I've emphasized in a number of places around countertransference, I think we're learning more and more the extent to which there are issues of health equity involved in all of this. And so, as part of the recognition of the irrationality of the prescribers, it's also important to recognize how our own unconscious biases may perpetuate or amplify systemic inequities. We know that there are pressures towards misdiagnosis in our patients of color.
References:
- Chien, P. L., & Bell, C. C. (2008). Racial differences and schizophrenia. Directions in Psychiatry, 28(4), 297-304.
- Schwartz, R. C., & Blankenship, D. M. (2014). Racial disparities in psychotic disorder diagnosis: A review of empirical literature. World Journal of Psychiatry, 4(4), 133.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 17 of 20
A number of studies have shown there is an increased likelihood that we're going to develop disempowering stances with patients from marginalized communities. We know, for example, statistically they're more likely to prefer counseling, but then we give them, as a whole, less information about treatment options and communicate with them in a way that perpetuates patient passivity. And we're more likely to prescribe oppressively in a way that, for example, those patients are much more likely to end up on higher doses of antipsychotics than patients from dominant social groups.
References:
- Segal, S. P., Bola, J. R., & Watson, M. A. (1996). Race, quality of care, and antipsychotic prescribing practices in psychiatric emergency services. Psychiatric Services (Washington, DC), 47(3), 282.
- Gordon, H. S., Street Jr, R. L., Sharf, B. F., & Souchek, J. (2006). Racial differences in doctors' information‐giving and patients' participation. Cancer, 107(6), 1313-1320.
- Lin, M. Y., & Kressin, N. R. (2015). Race/ethnicity and Americans’ experiences with treatment decision making. Patient Education and Counseling, 98(12), 1636-1642.
Slide 18 of 20
In summary: Patients with overwhelming affects very often induce corresponding affects in others. We can then prescribe in efforts not to address the patient's anxiety but to address our own, and this can lead to irrational prescribing. When patients bring transference-based negative preconceptions into care about treatment, it is typically important to identify this and address it before, or if you can, or when it becomes a source of treatment resistance.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 19 of 20
There is an increased likelihood that countertransference factors outweigh rational decision-making in the prescription of medications. These things may be operating in us outside of our awareness. As part of the recognition of the irrationality of the prescribers, it's also important to recognize how our own unconscious biases may perpetuate or amplify systemic inequities.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.