Slides and Transcript
Slide 2 of 11
Bulimia nervosa is characterized by recurrent episodes of binge eating. It’s true that a binge involves eating an amount of food that is definitely larger than what most individuals would eat in a similar period of time. But that’s very subjective and somewhat judgmental. What’s most important in terms of making a binge a binge is the sense of lack of control. We all may overeat at certain times like at buffets at conferences, holidays or birthdays but we don’t have that loss of control that is required for it to be considered a binge. It’s the feeling that one just cannot stop eating or control what and how much one is eating.
References:
- American Psychiatric Association. (2013). Feeding and eating disorders. In Diagnostic and Statistical Manual of Mental Disorders (5th ed.).
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 3 of 11
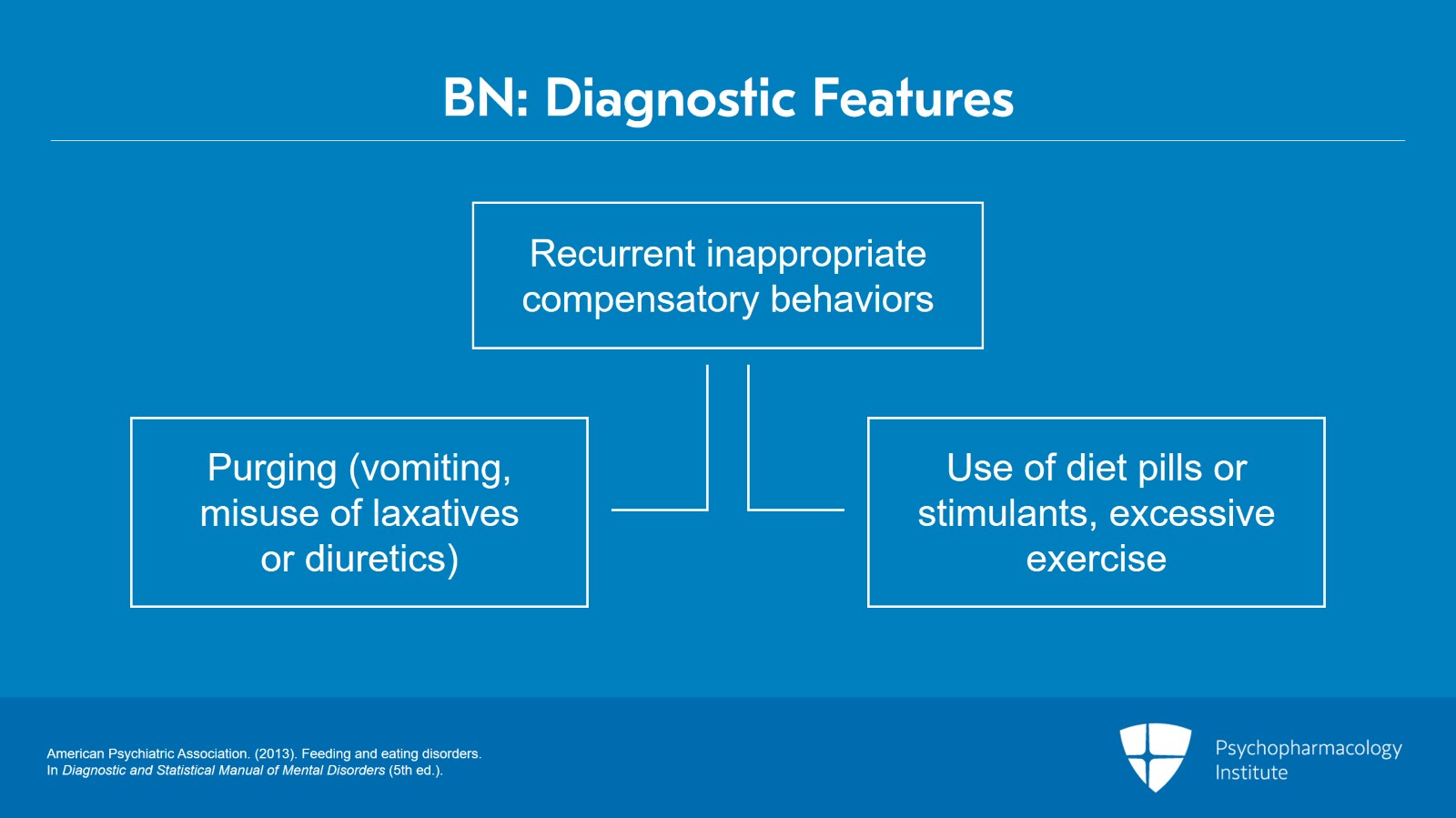
And along with these recurrent episodes of binge eating, there are recurrent inappropriate compensatory behaviors, usually purging behaviors. Now, purging technically means self-induced vomiting, misuse of laxatives or diuretics. The use of diet pills or stimulants, excessive exercise are indeed compensatory behaviors but they are technically not purging behaviors.
References:
- American Psychiatric Association. (2013). Feeding and eating disorders. In Diagnostic and Statistical Manual of Mental Disorders (5th ed.).
Slide 4 of 11
In addition, self-evaluation is unduly influenced by body size or shape. And the disorder does not occur exclusively during episodes of anorexia nervosa. And then similarly with anorexia nervosa, there is a partial and full remission specification. And then the severity specification is based on the number of episodes per week from just requiring one time per week in mild cases to 14 or more times per week in extreme cases.
References:
- American Psychiatric Association. (2013). Feeding and eating disorders. In Diagnostic and Statistical Manual of Mental Disorders (5th ed.).
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 5 of 11
I have seen many cases of bulimia nervosa in which the person is literally bingeing and vomiting all day long every day. They tend to go from one fast food restaurant to another, stopping in the bathrooms to self-induce vomit. Clinicians should have a high index of suspicion about the presence of bulimia nervosa especially in women who manifest high levels of psychiatric comorbidity, suicidality and electrolyte disturbances.
Slide 6 of 11
The history of pharmacological treatments that had been studied goes back to the 1980s when a variety of antidepressants whether tricyclic antidepressants, MAO inhibitor antidepressants or SRIs, serotonin reuptake inhibitors, have been found to be helpful in the acute treatment of bulimia nervosa. Fluoxetine has also been shown to be effective in the maintenance treatment of bulimia nervosa.
References:
- Zhu, A. J., & Walsh, B. T. (2002). Pharmacologic treatment of eating disorders. Canadian Journal of Psychiatry. Revue Canadienne de Psychiatrie, 47(3), 227–234.
- Romano, S. J., Halmi, K. A., Sarkar, N. P., Koke, S. C., & Lee, J. S. (2002). A placebo-controlled study of fluoxetine in continued treatment of bulimia nervosa after successful acute fluoxetine treatment. The American Journal of Psychiatry, 159(1), 96–102.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 7 of 11
Please note that although bupropion was found to be superior to placebo there was an inordinately higher risk of grand mal seizures and there is a black box warning against the use of bupropion in eating disorders. I would strongly recommend do not use bupropion in patients with eating disorders. You may very well have patients come to you on bupropion. But when they come to me, I taper them off of it. I explain why. Because medicolegally you don’t stand a prayer if something would happen. If that person were driving, for example, and had a seizure and you’ve been prescribing bupropion, bad news. There are plenty of other treatments that can be helpful besides bupropion.
References:
- Israël M. (2002). Should some drugs be avoided when treating bulimia nervosa?. Journal of Psychiatry and Neuroscience, 27(6), 457.
Slide 8 of 11
There is one small study with trazodone but it’s not something that I use given its side effects especially at higher doses. There is evidence for topiramate, also difficult to tolerate. And there is the antiemetic I mentioned previously, ondansetron. I’m going to show you the results of all of these studies.
References:
- Hoopes, S. P., Reimherr, F. W., Hedges, D. W., Rosenthal, N. R., Kamin, M., Karim, R., Capece, J. A., & Karvois, D. (2003). Treatment of bulimia nervosa with topiramate in a randomized, double-blind, placebo-controlled trial, part 1: improvement in binge and purge measures. The Journal of Clinical Psychiatry, 64(11), 1335–1341.
- Faris, P. L., Kim, S. W., Meller, W. H., Goodale, R. L., Oakman, S. A., Hofbauer, R. D., Marshall, A. M., Daughters, R. S., Banerjee-Stevens, D., Eckert, E. D., & Hartman, B. K. (2000). Effect of decreasing afferent vagal activity with ondansetron on symptoms of bulimia nervosa: a randomised, double-blind trial. Lancet, 355(9206), 792–797.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 9 of 11
The key points here are: Objective binge eating is defined by not only eating a large amount of food in a discrete period of time but most importantly a subjective sense of lack of control over eating. The presence of compensatory behavior distinguishes bulimia nervosa from binge eating disorder.
Slide 10 of 11
The mainstay of treatment of bulimia nervosa is antidepressants especially fluoxetine at higher doses, for example, 60 to 80 mg per day but other agents such as topiramate and ondansetron have also been found effective.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.