Slides and Transcript
Slide 1 of 16
Now, let’s turn to another class of medications, antipsychotics, and their use during breastfeeding.
Slide 2 of 16
I’m going to begin to sound a little bit like a broken record here because the first point I want to make is that there are more data about older drugs, which is the same thing I said about antidepressants.
First-generation antipsychotics have been well studied. They generally have a low milk-to-plasma ratio and are considered compatible with breastfeeding.
Most second-generation antipsychotics are also considered compatible with breastfeeding, but we have fewer data because they’re newer drugs.
References:
- Uguz, F. (2016). Second-generation antipsychotics during the lactation period. Journal of Clinical Psychopharmacology, 36(3), 244-252.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 3 of 16
A few things to know about some of the second-generation antipsychotics though since those are used so commonly. Aripiprazole may actually suppress prolactin levels so milk supply could be a concern. It doesn’t mean you can’t use it, but it means you have to watch out for that milk supply. And in particular, it may be tricky to use in very early stages when breastfeeding is just getting going and supply is just being established.
Risperidone and several other agents may increase prolactin which would actually benefit milk supply so no problems there.
References:
- Uguz, F. (2016). Second-generation antipsychotics during the lactation period. Journal of Clinical Psychopharmacology, 36(3), 244-252.
- Pacchiarotti, I., León-Caballero, J., Murru, A., Verdolini, N., Furio, M. A., Pancheri, C., Valentí, M., Samalin, L., Roigé, E. S., González-Pinto, A., Montes, J. M., Benabarre, A., Crespo, J. M., De Dios Perrino, C., Goikolea, J. M., Gutiérrez-Rojas, L., Carvalho, A. F., & Vieta, E. (2016). Mood stabilizers and antipsychotics during breastfeeding: Focus on bipolar disorder. European Neuropsychopharmacology, 26(10), 1562-1578.
Slide 4 of 16
Quetiapine is the one that has the lowest passage into the breastmilk due to the large size of the molecule. So, this is the reason that I mentioned that anecdote before about somebody refusing to let a woman breastfeed because she was on quetiapine. And actually, of all the second-generation antipsychotics, it’s the one that’s going to get into the breastmilk the least.
One exception to compatibility in breastfeeding for second-generation antipsychotics is clozapine and we’re going to talk a little bit more about that later.
References:
- Uguz, F. (2016). Second-generation antipsychotics during the lactation period. Journal of Clinical Psychopharmacology, 36(3), 244-252.
- Pacchiarotti, I., León-Caballero, J., Murru, A., Verdolini, N., Furio, M. A., Pancheri, C., Valentí, M., Samalin, L., Roigé, E. S., González-Pinto, A., Montes, J. M., Benabarre, A., Crespo, J. M., De Dios Perrino, C., Goikolea, J. M., Gutiérrez-Rojas, L., Carvalho, A. F., & Vieta, E. (2016). Mood stabilizers and antipsychotics during breastfeeding: Focus on bipolar disorder. European Neuropsychopharmacology, 26(10), 1562-1578.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 5 of 16
There’s also no information about the newest antipsychotic drugs like brexpiprazole and cariprazine. We just don’t have any data. Chances are we will eventually show that those are also compatible because there’s no reason to expect them to have different risks than the drugs that we know something about, but the reality is we know nothing about them. And it’s always important to use a drug about which you have more data.
References:
- Uguz, F. (2016). Second-generation antipsychotics during the lactation period. Journal of Clinical Psychopharmacology, 36(3), 244-252.
- Pacchiarotti, I., León-Caballero, J., Murru, A., Verdolini, N., Furio, M. A., Pancheri, C., Valentí, M., Samalin, L., Roigé, E. S., González-Pinto, A., Montes, J. M., Benabarre, A., Crespo, J. M., De Dios Perrino, C., Goikolea, J. M., Gutiérrez-Rojas, L., Carvalho, A. F., & Vieta, E. (2016). Mood stabilizers and antipsychotics during breastfeeding: Focus on bipolar disorder. European Neuropsychopharmacology, 26(10), 1562-1578.
Slide 6 of 16
So, let’s talk a little bit more about clozapine. Clozapine is actually the only psychiatric drug that’s nearly always contraindicated in breastfeeding and the reason for that is that the risk for agranulocytosis is just too great.
References:
- Mehta, T. M., & Van Lieshout, R. J. (2016). A review of the safety of clozapine during pregnancy and lactation. Archives of Women's Mental Health, 20(1), 1-9.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 7 of 16
If used, you have to monitor the infant for sedation and you would also have to monitor the white blood cell count regularly and that is too high a bar for most parents and pediatricians to be on board with. So that risk is just too great. And most women who have to take clozapine would be advised not to breastfeed for that reason.
References:
- Mehta, T. M., & Van Lieshout, R. J. (2016). A review of the safety of clozapine during pregnancy and lactation. Archives of Women's Mental Health, 20(1), 1-9.
Slide 8 of 16
So, let’s look at a case vignette for use of antipsychotic. This time, we’re going to talk about Ana Q. She is a 26-year-old with paranoid schizophrenia. She’s had two prior hospitalizations.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 9 of 16
She was stable for over six months prior to her pregnancy.
She has a supportive partner and family and she’s extremely committed to breastfeeding.
Slide 10 of 16
She’s had good response in the past to aripiprazole, lurasidone, and risperidone and she was taking risperidone during her pregnancy and remained asymptomatic.
She is very concerned about weight gain effects of these drugs that’s been a problem for her in the past.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 11 of 16
Her baby was born at 38 weeks, has a healthy birth weight and mature liver function, was fed formula in the hospital because the nurses were concerned about the mother’s medications and the mother is quite upset about this.
Slide 12 of 16
Remember that using what’s worked for the mother in the past is a very important factor.
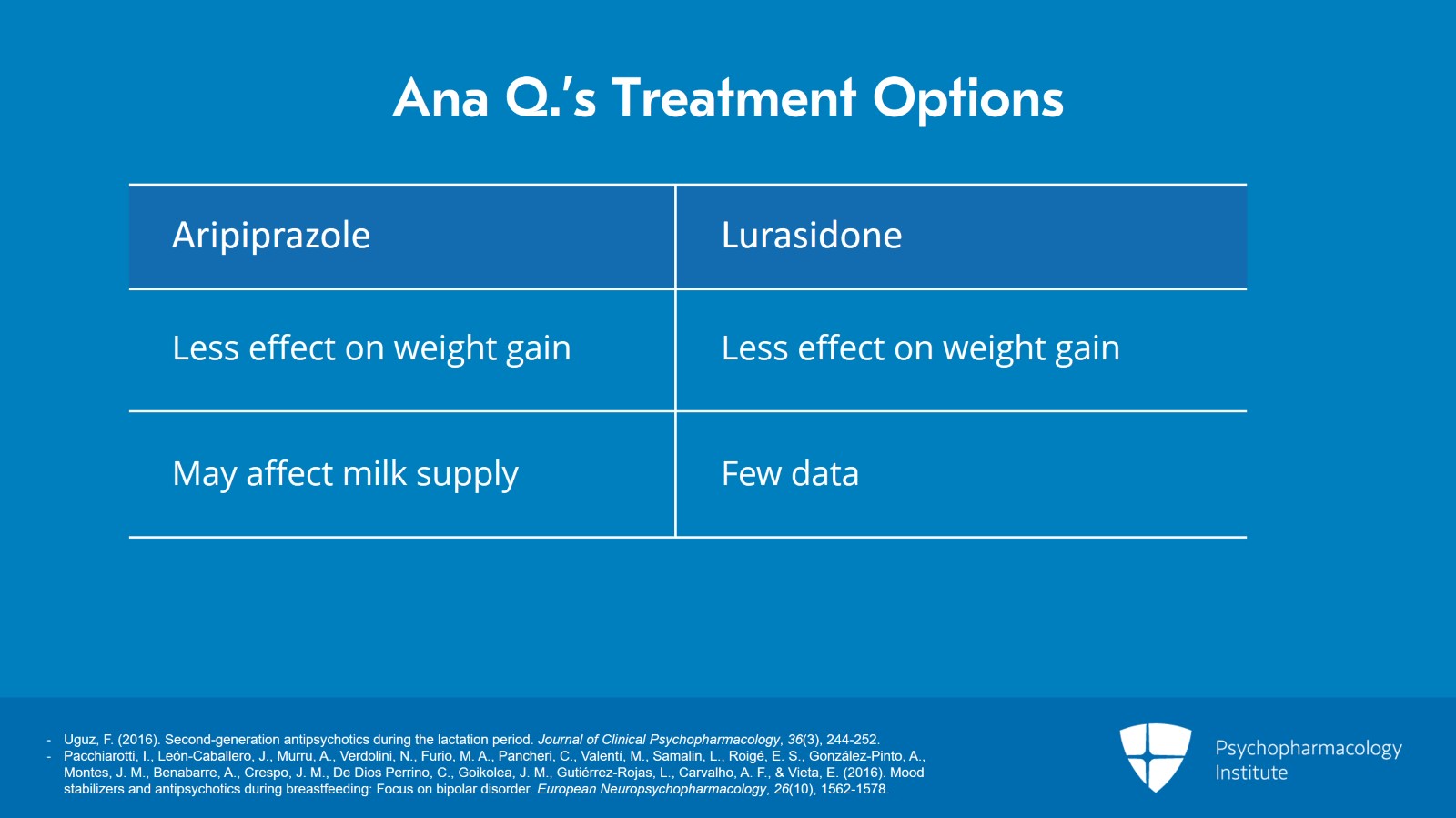
In this case, aripiprazole and lurasidone are likely to have less effect on weight which is a big concern for her, but we have few data on lurasidone, and we know that aripiprazole may affect milk supply.
In fact, this mother is also one step behind in milk supply because the baby has been fed formula in the hospital and she didn’t have that sensory stimulation of the newborn sucking.
References:
- Pacchiarotti, I., León-Caballero, J., Murru, A., Verdolini, N., Furio, M. A., Pancheri, C., Valentí, M., Samalin, L., Roigé, E. S., González-Pinto, A., Montes, J. M., Benabarre, A., Crespo, J. M., De Dios Perrino, C., Goikolea, J. M., Gutiérrez-Rojas, L., Carvalho, A. F., & Vieta, E. (2016). Mood stabilizers and antipsychotics during breastfeeding: Focus on bipolar disorder. European Neuropsychopharmacology, 26(10), 1562-1578.
- Mendhekar, D., Sunder, K. R., & Andrade, C. (2006). Aripiprazole use in a pregnant schizoaffective woman. Bipolar Disorders, 8(3), 299-300.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 13 of 16
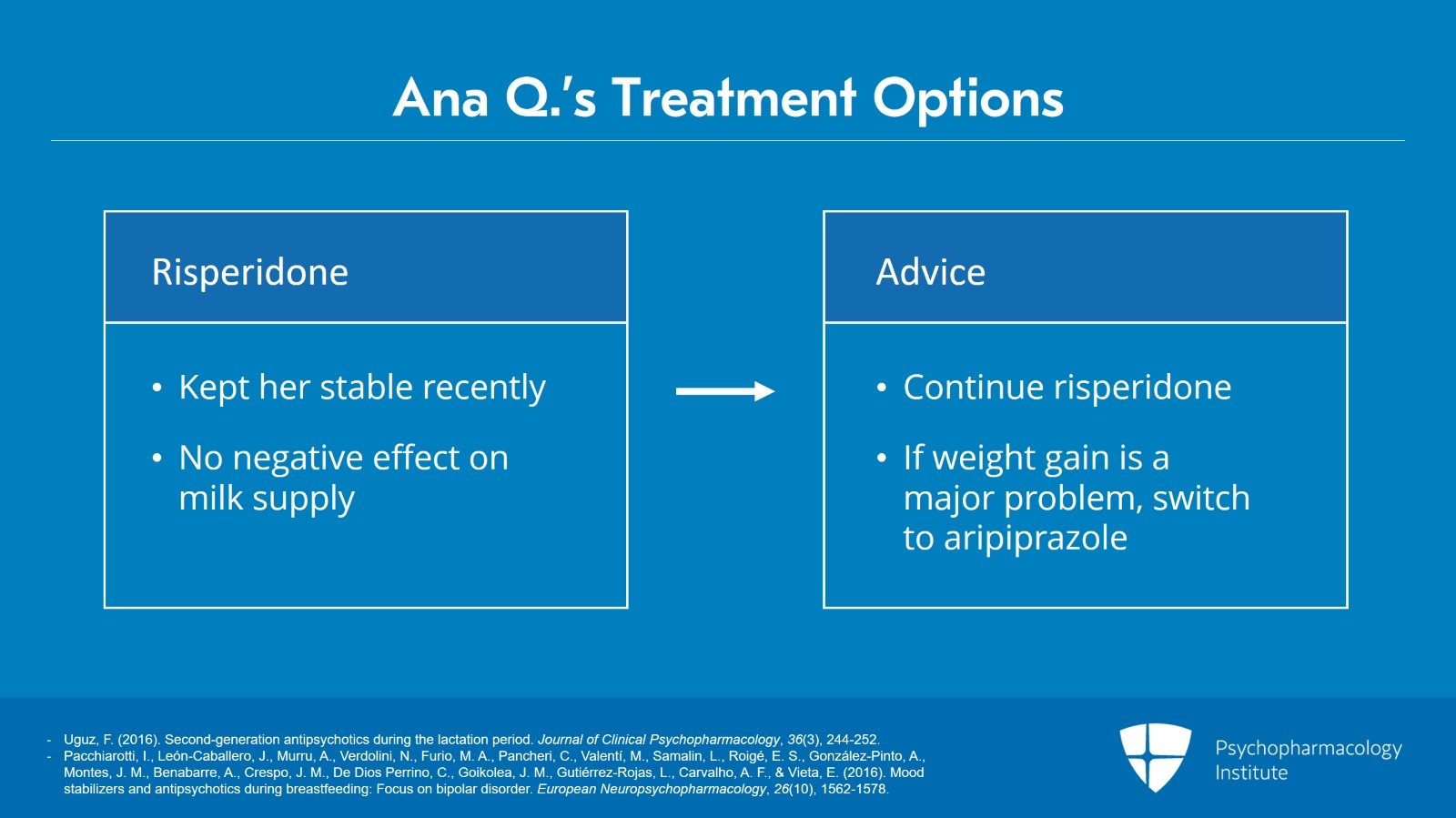
As risperidone has kept her stable recently and wouldn’t have a negative effect on milk supply, the advice would be to continue risperidone.
If weight gain becomes a major issue, she can consider a switch to aripiprazole down the road once milk production is well established.
References:
- Uguz, F. (2016). Second-generation antipsychotics during the lactation period. Journal of Clinical Psychopharmacology, 36(3), 244-252.
- Pacchiarotti, I., León-Caballero, J., Murru, A., Verdolini, N., Furio, M. A., Pancheri, C., Valentí, M., Samalin, L., Roigé, E. S., González-Pinto, A., Montes, J. M., Benabarre, A., Crespo, J. M., De Dios Perrino, C., Goikolea, J. M., Gutiérrez-Rojas, L., Carvalho, A. F., & Vieta, E. (2016). Mood stabilizers and antipsychotics during breastfeeding: Focus on bipolar disorder. European Neuropsychopharmacology, 26(10), 1562-1578.
Slide 14 of 16
So, what are the key points for this section on antipsychotics in breastfeeding?
First-generation antipsychotics are considered compatible with breastfeeding.
The same is true for most second-generation antipsychotics but we have no data on the newest drugs, for example, brexpiprazole and cariprazine.
It’s always better to use an older drug with more data if it’s possible to keep the mother well that way.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.
Slide 15 of 16
Remember that keeping the mother well is paramount.
And the one antipsychotic that’s nearly always contraindicated in breastfeeding is clozapine due to the risk for agranulocytosis.
Free Files
Download PDF and other files
Success!
Check your inbox, we sent you all the materials there.